-
Depression is increasingly considered a public health problem; the total number of people living with depression worldwide in 2015 was 322 million, with a prevalence of 7.5% among females aged 55–74, and 5.5% among males[1]. Depression can lead to disability and cognitive decline and affect the quality of life of older adults[2]. Depressive disorders were the second leading cause of years lived with disability in 2010, and a leading cause of disability adjusted of life years [3]. Several lifestyle factors have been associated with depression, including poor diet [4], lack of physical activity [5], and obesity [6]. Notably, obesity is a major public health problem in China, and the latest national prevalence estimates for 2015 to 2019, based on criteria in China, were 34.3% for overweight adults and 16.4% for obese adults [7]. Several studies have investigated the association between obesity and depression in older adults, showing that obesity increases the incidence of depressive symptoms in older adults [8] and that initial levels of body mass index (BMI) and depressive symptoms correlate positively with each other [9]. However, findings on the relationship between obesity and depressive symptoms are inconsistent, and some studies have suggested that obesity or high BMI are protective factors for depression [10, 11]. In addition, the association between obesity and depression in older Chinese adults remains unclear.
The systemic inflammatory response is considered an important biological mechanism in the relationship between obesity and depression [12]. Chronic low-grade inflammation is a hallmark of obesity and a central pathophysiological process in depression [13]. High levels of C-reactive protein (CRP), a chronic marker of systemic inflammation [14], are associated with depression and high BMI [15]. However, some studies have suggested that the effect of systemic inflammation on depression is symptom-specific: positive for physical symptoms and negative for emotional symptoms [16].
To address these knowledge gaps, we investigated the association of obesity with depression in older adults and explored the role of systemic inflammation defined by CRP in this relationship using the Longitudinal Study of Disability and Cognitive Impairment.
-
Participants in this study were ≥ 65 years old, from the study of Surveillance and Management of Disability and Cognitive Impairment in older adults (SUM-DCI), which was established in 2018. One district/city each was selected from Liaoning province and Xinjiang Urgur Autonomous Region. In each district, two towns/streets were selected, where 500 subjects from each were recruited. A total of 1,973 subjects participated in the baseline survey, among which 1,459 were followed up in 2021.
The SUM-DCI study was approved by the Ethics Committee of the Chinese Center for Disease Control and Prevention. Written informed consent was obtained from all participants (or their proxies).
-
Depression was assessed using the geriatric depression scale-15 (GDS-15), a 15-item validated self-report questionnaire commonly used to measure depression in older adults [17], at baseline and at follow-up. Depression was defined as “yes” if the GDS score was ≥ 5 [18], and the change in the GDS score between baseline and follow-up was calculated; the highest quartile of change (≥ 2 points increase in GDS score) was defined as “worsening depressive symptoms” [19].
GDS-15 can be explained by three sub-dimensions, including general depressive affect [general depressive affect (GDA), seven items], life satisfaction [life satisfaction (LS), four items], and withdrawal [withdrawal (W), three items], with one item of “memory problems” omitted because it attributed to the aging process [20]. The detailed items for the GDA were as follows: 1) life is empty; 2) often get bored; 3) afraid something bad will happen; 4) often feeling helpless; 5) feeling worthless; 6) situation is hopeless; and 7) most people are better off than you are. The items included in LS are as follows: 1) satisfied with life; 2) in good spirits; 3) happy most of the time; and 4) wonderful to be alive now. The items for W were as follows: 1) dropped activities and interests; 2) preferred to stay at home; and 3) feeling full of energy.
-
Weight, height, and waist circumference (WC) were measured twice using standard methods, BMI was calculated as weight in kilograms divided by height in meters squared. General obesity was defined as a BMI ≥ 28.0, overweight as 24 ≤ BMI < 28.0, normal weight as 18.5 ≤ BMI < 24.0, and underweight as BMI ≤ 18.5. Abdominal obesity was defined using waist circumference, considering the criterion of ≥ 90 cm for males and ≥ 85 cm for females [21].
-
Chronic systemic inflammation was assessed using high-sensitivity CRP (hs-CRP). Fasting venous blood samples were collected, and serum was used to assess the baseline levels of hs-CRP and fasting plasma glucose (FPG) using a commercially available diagnostic kit (Roche Diagnostics, Mannheim, Germany) with an Automatic Biochemistry Analyzer (Hitachi 7180, Japan). High level of hs-CRP was defined as hs-CRP > 3 mg/L [22, 23].
The covariates included sociodemographics (age, sex, education level, marital status, living arrangement, and home income), lifestyle (smoking, exercise, and tea drinking), social activities, diabetes, hypertension, and sleep disturbance. Living arrangements were classified as “living alone” or not. Marital status was dichotomized as “yes” if the participant was currently married, and “no” if they were divorced, widowed, or never married. Social activity was assessed by asking the following questions: 1) How often did you do the following activities: a) going for outdoor activities and b) joining organized activities? The answers were measured on a scale from 1 to 5, such that: 1, almost everyday; 2, not every day but ≥ 1 time/week; 3, < 1 time/week but ≥ 1 time/month; 4, sometimes; and 5, never. We dichotomized responses for the above individual activities into two categories: “yes” if the answer was “almost every day” or “not every day but ≥ 1 time/week”, and “no” if the answer was any of the remaining activity levels; 2) “How many times did you travel in the past two years?” were defined as “yes” if the answer was once or more. A positive answer to any of the three types of social activities was coded as “yes.” High income was defined as a high tertile of home income per year. Systolic blood pressure (SBP) and diastolic blood pressure (DBP) were measured twice using the right arm, and the mean values were used. Hypertension was defined when SBP was ≥ 140 mmHg and/or DBP was ≥ 90 mmHg and/or self-reported diagnosis in hospital. Diabetes was defined as FPG ≥ 7.0 mmol/L and/or self-reported diagnosis in hospital [24]. Participants reported their sleep symptoms during the last month for at least 3 days each week, using the following questions: 1) “Taking > 30 min to fall asleep after going to bed?” (difficulty in initiating sleep); 2) “Waking up in the middle of the night two times or more?” (difficulty in maintaining sleep); and 3) “Waking up early and not being able to go back to sleep?” (early-morning waking), and sleep disturbance was defined if any response to the questions above was “yes” [25].
-
Participant characteristics by follow-up status and sex were compared using chi-square tests for categorical variables and t-tests for continuous variables, except for scores of GDS, GDA, LS, and W, which were all skewed distributed and shown as median values (M) and interquartile ranges (IQR). The four scores by follow-up status and sex were compared using Wilcoxon rank-sum non-parametric tests. The number of underweight participants was quite small (n = 30); therefore, underweight participants were not included in subsequent statistical analysis, which meant that the final sample size in subsequent statistical analysis was 1,429 of whom 1,085 subjects were free of depression at baseline. To explore the association between obesity and depression, logistic regression was used to analyze the odds ratio (OR) and 95% confidence interval (CI) of obesity for worsening depressive symptoms and incident depression. Three models were fit as follows: Model 1 was adjusted for baseline GDS score alone; Model 2 was further adjusted for age, sex, education level, marital status, living alone, and home income; and Model 3 was further adjusted for smoking, exercise, tea drinking, social activities, diabetes, hypertension, and sleep disturbance. The associations between obesity and depression among male and female participants were explored using logistic regression analysis.
To explore the possible role of CRP in the association between obesity and depression, we first explored the association between obesity and CRP levels using logistic regression, in which high CRP levels were used as dependent variables. We further explored the associations of CRP levels at baseline (independent variable) with GDS score and the scores of its three dimensions (GDA, LS, and W) at follow-up, as well as with score differences between baseline and follow-up, using linear regression models in which scores of GDS, GDA, LS, and W were transformed to log (1+Y) when scores at follow-up were investigated, and CRP level was transformed to log (X), considering of the skewed distribution of these variables. Data were shown as β (95% CI), representing change of log (1+Y) or Difference between baseline and follow-up for one unit of log (X). Notably, age, sex, education level, marital status, smoking, exercise, tea drinking, social activities, diabetes, hypertension, and sleep disturbance were adjusted for.
All statistical analyses were performed using SAS, version 9.4 (SAS Institute Inc., Cary, NC, USA). P < 0.05 was considered statistically significant; all P-values were two-sided.
-
The characteristics of the participants by followed up status and sex are listed in Table 1. No significant difference was observed between the subjects who were followed up and those who were lost, except that those who were lost to follow-up had fewer years of education and a slightly higher GDS score. Among the followed up subjects, compared with female participants, male participants were more likely to be educated, married, and wealthy, and usually reported a high prevalence of smoking and tea drinking, more social activities, and a lower prevalence of hypertension, sleep disturbance, and living alone.
Characteristics Total Followed up Lost Male Female P-value No. of subjects 1,459 605 854 514 Age (years), mean (SD) 70.94 (4.24) 71.27 (4.31) 70.70 (4.17) 0.01 71.10 Education years* 0 202 (13.85) 42 (6.94) 160 (18.74) < 0.001 99 (19.26) 1–6 478 (32.76) 185 (30.58) 293 (34.31) 166 (32.30) > 6 779 (53.39) 378 (62.48) 401 (46.96) 249 (48.44) Married 1,118 (76.63) 553 (91.40) 565 (66.16) < 0.001 382 (74.32) Living alone 214 (14.67) 47 (7.77) 167 (19.56) < 0.001 85 (16.54) High income 513 (35.16) 240 (39.67) 273 (31.97) 0.002 164 (31.91) Smoking 190 (13.02) 187 (30.91) 3 (0.35) < 0.001 79 (15.37) Tea drinking 219 (15.01) 147 (24.30) 72 (8.43) < 0.001 61 (11.87) Exercise 1,043 (71.49) 434 (71.74) 609 (71.31) 0.86 372 (72.37) Social activities 1,334 (91.43) 567 (93.72) 767 (89.81) 0.009 465 (90.47) Hypertension 611 (41.88) 221 (36.53) 390 (45.67) 0.0005 203 (39.49) Diabetes 258 (17.68) 101 (16.69) 157 (18.38) 0.40 97 (18.87) Sleep disturbance 772 (52.91) 280 (46.28) 492 (57.61) < 0.001 264 (51.36) General obesity Underweight 30 (2.06) 11 (1.82) 19 (2.22) 0.66 19 (3.70) Normal weight 479 (32.83) 196 (32.40) 283 (33.14) 0.49 172 (33.46) Overweight 650 (44.55) 280 (46.28) 370 (43.33) 215 (41.83) Obesity 300 (20.56) 118 (19.50) 182 (21.31) 108 (21.01) Abdominal obesity 791 (54.22) 323 (53.39) 468 (54.80) 0.59 281 (54.67) Baseline scores GDS* 2 (1, 4) 2 (1, 4) 2 (1, 5) 0.22 3 (1, 5) GDA 0 (0, 1) 0 (0, 1) 0 (0, 2) 0.005 0 (0, 2) LS 1 (1, 1) 1 (1, 1) 1 (1, 1) 0.31 1 (1, 1) W 0 (0, 1) 0 (0, 1) 0 (0, 1) 0.15 1 (0, 1) Follow-up scores GDS 3 (2, 5) 3 (2, 5) 3 (2, 5) 0.34 − GDA 1(0, 2) 1 (0, 2) 1 (0, 2) 0.08 − LS 1 (1.1) 1 (1, 1) 1 (1, 1) 0.40 − W 1 (0.1) 1 (0, 1) 1 (0, 1) 0.60 − Note. Data were shown as n (%) for categorical variables and as x (s) for continuous variables. *The difference between the subjects who were followed up and those lost to follow-up was statistically significant (P < 0.05). The GDS, GDA, LS, and W scores were shown as M (IQR). GDS, geriatric depression scale; GDA, general depressive affect; LS, life satisfaction; W, withdrawal. Table 1. Characteristics of study participants by psychological resilience status
Compared with the group of normal weight, those obesity subjects were significantly more likely to have “worsening depressive symptoms,” with OR (95% CI) of 1.42 (1.02–1.98); among those depression-free participants at baseline, the risk of incident depression at follow-up was also significantly increased, with OR (95% CI) of 1.65 (1.10–2.47). However, abdominal obesity was not statistically associated with the worsening of depressive symptoms or the incidence of depression (Table 2).
Obesity status Model 1 Model 2 Model 3 Worsen depressive symptoms (n = 1,429) General obesity Normal weight 1.00 (reference) 1.00 (reference) 1.00 (reference) Overweight 1.00 (0.76, 1.30) 0.98 (0.75, 1.29) 0.97 (0.74, 1.29) Obesity 1.53 (1.13, 2.12)** 1.43 (1.03, 1.97)* 1.42 (1.02, 1.98)* Abdominal obesity No 1.00 (reference) 1.00 (reference) 1.00 (reference) Yes 1.13 (0.86, 1.47) 1.08 (0.83, 1.42) 1.10 (0.83, 1.44) Incident depression (n = 1,085) General obesity Normal weight 1.00 (reference) 1.00 (reference) 1.00 (reference) Overweight 1.09 (0.78, 1.51) 1.06 (0.76, 1.49) 1.05 (0.75, 1.48) Obesity 1.80 (1.23, 2.63)** 1.68 (1.14, 2.47)** 1.65 (1.10, 2.47)** Abdominal obesity No 1.00 (reference) 1.00 (reference) 1.00 (reference) Yes 1.05 (0.76, 1.45) 0.99 (0.71, 1.38) 0.99 (0.71, 1.39) Note. *P < 0.05, **P < 0.01. Model 1: adjusted for baseline GDS score alone; Model 2: additionally adjusted for age, sex, education level, marital status, living alone, and home income; and Model 3: further adjusted for smoking, exercise, tea drinking, social activities, diabetes, hypertension, and sleep disturbance. Table 2. Association of obesity with worsen depressive symptom and incident depression
We further conducted analyses among male and female subjects separately and observed that the association of general obesity with worsening depressive symptoms and incident depression existed in male participants alone, with OR (95% CI) of 2.08 (1.27–3.42) and 2.12 (1.20–3.74), respectively. However, abdominal obesity was not significantly associated with depression in either sex (Table 3).
Obesity status Male Female Model 1 Full model Model 1 Full model Worsening depressive symptoms General obesity Normal weight 1.00 (reference) 1.00 (reference) 1.00 (reference) 1.00 (reference) Overweight 1.38 (0.92, 2.08) 1.42 (0.93, 2.19) 0.78 (0.55, 1.10) 0.73 (0.51, 1.06) Obesity 2.08 (1.27, 3.42)** 2.12 (1.25, 3.58)* 1.24 (0.82, 1.89) 1.05 (0.67, 1.64) Abdominal obesity No 1.00 (reference) 1.00 (reference) 1.00 (reference) 1.00 (reference) Yes 1.10 (0.74, 1.63) 1.08 (0.72, 1.63) 1.14 (0.80, 1.63) 1.11 (0.76, 1.62) Incident depression General obesity Normal weight 1.00 (reference) 1.00 (reference) 1.00 (reference) 1.00 (reference) Overweight 1.05 (0.64, 1.74) 1.07 (0.63, 1.81) 1.11 (0.72, 1.72) 1.04 (0.66, 1.65) Obesity 2.12 (1.20, 3.74)** 2.24 (1.22,4.11)** 1.56 (0.93, 2.61) 1.24 (0.71, 2.15) Abdominal obesity No 1.00 (reference) 1.00 (reference) 1.00 (reference) 1.00 (reference) Yes 1.01 (0.63, 1.62) 1.01 (0.62, 1.67) 1.09 (0.70, 1.70) 1.02 (0.64, 1.63) Note. Data were presented as OR (95% CI). Model 1: adjusted for baseline GDS score alone; Full model: additionally adjusted for age, sex, education level, marital status, living alone, home income, smoking, exercise, tea drinking, social activities, diabetes, hypertension, and sleep disturbances. *P < 0.05, **P < 0.01. Table 3. Association of obesity with worsening depressive symptoms and incident depression among male and female participants
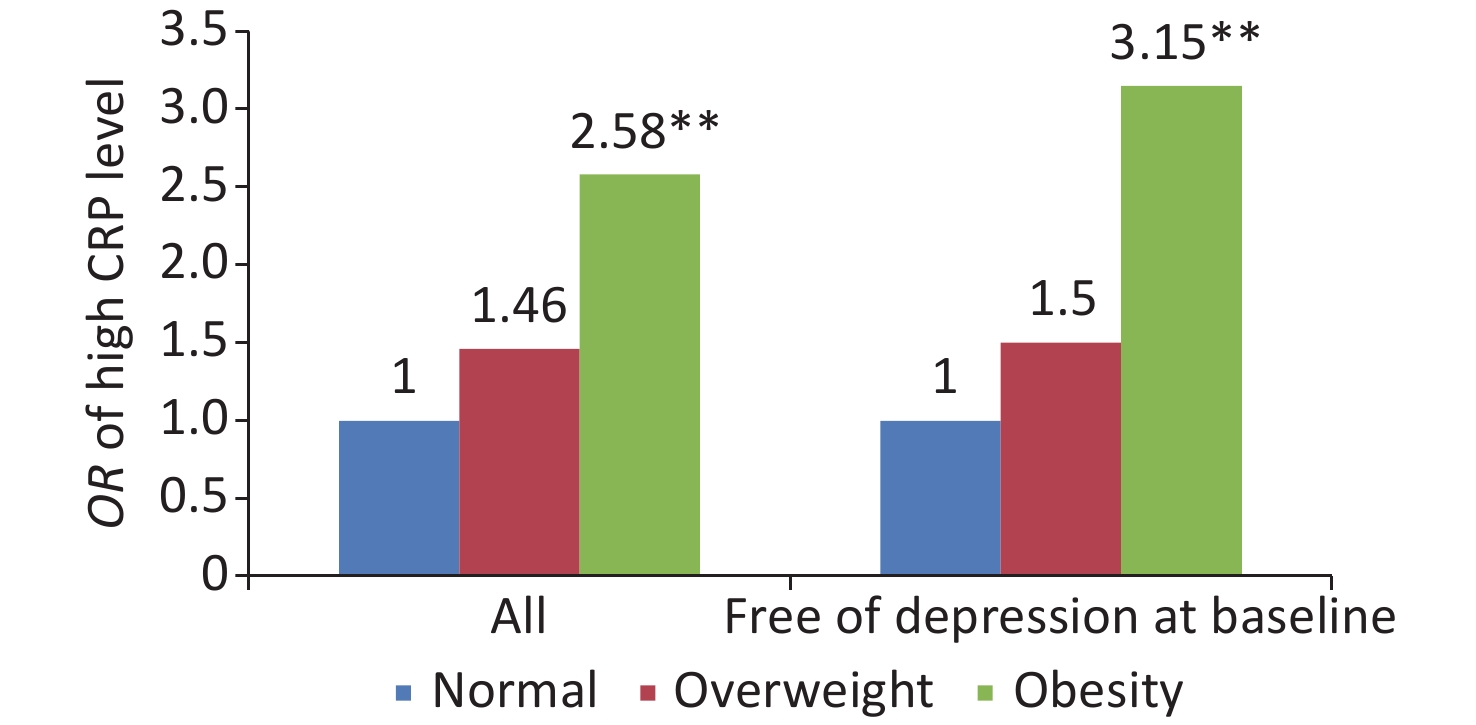
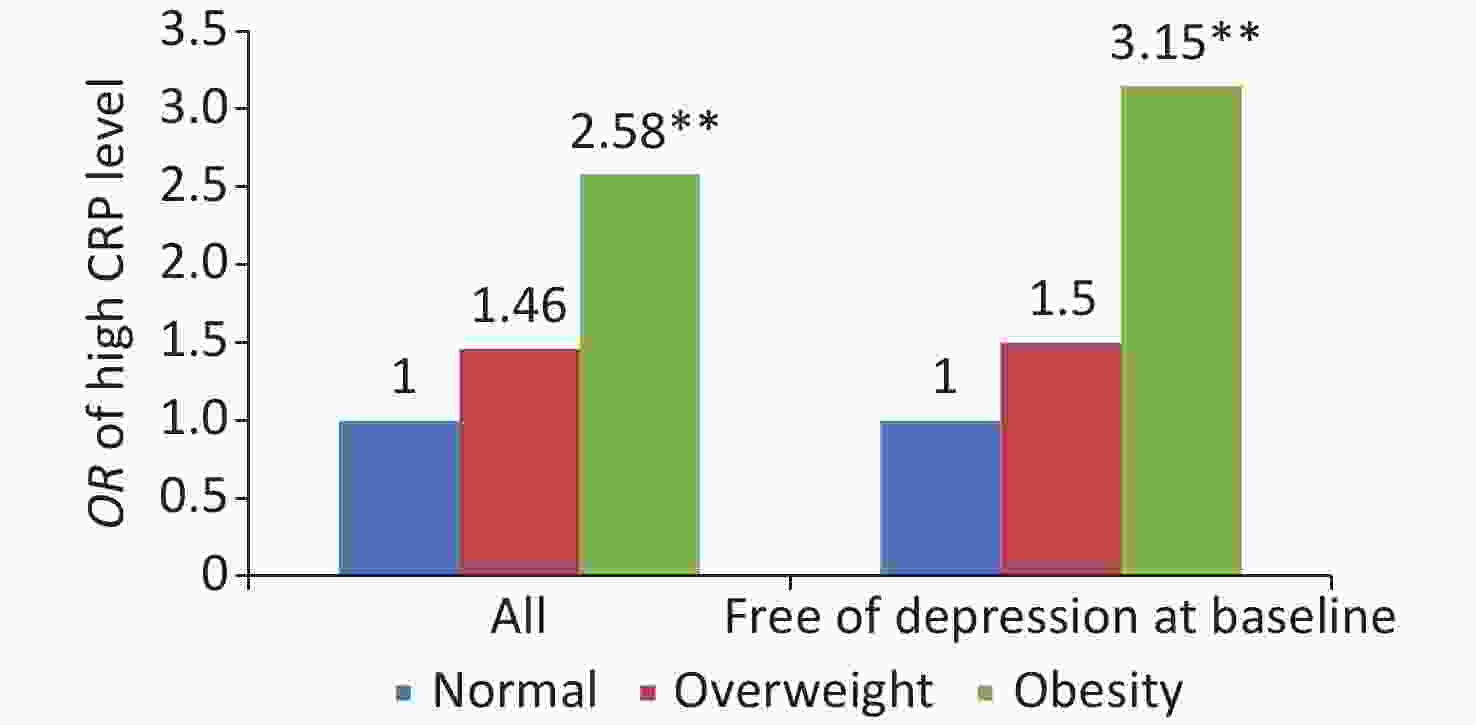
Analysis revealed that general obesity was associated with high level of CRP (Linear trend, P < 0.001), with OR (95% CI) of 2.58 (1.75–3.81) in all the followed up subjects, and among the participants free of depression at baseline, the results were consistent, with OR (95% CI) of 3.15 (1.97–5.04) (Figure 1).
The results revealed that the baseline CRP levels were not significantly associated with the GDS score at follow-up (P > 0.05) or with the score difference between baseline and follow-up (P > 0.05). However, it was significantly positively related with LS score (P < 0.05), specific dimension of depression, with β (95% CI) of was 0.015 (0.001, 0.03) and 0.018 (0.002, 0.03) among all participants and subjects free of depression at baseline, respectively, for score at follow-up; and for score difference between baseline and follow-up, the β was 0.04. No significant associations were observed between the CRP levels and GDA or W (Table 4).
GDS and
dimensionsScore at follow-up Difference between baseline and follow-up All followed up Free of depression at baseline All followed up Free of depression at baseline GDS 0.003 (−0.02,0.03) 0.001 (−0.03, 0.03) −0.012 (−0.16, 0.13) −0.010 (−0.16, 0.14) GDA −0.002 (−0.03, 0.03) −0.005 (−0.04, 0.03) 0.039 (−0.003, 0.08) 0.034 (−0.009, 0.08) LS 0.015 (0.001, 0.03)* 0.018 (0.002, 0.03)* 0.038 (0.006, 0.07)* 0.039 (0.005, 0.07)* W −0.016 (−0.04, 0.01) −0.022 (-0.05, 0.01) −0.028 (−0.07, 0.02) −0.036 (−0.08, 0.01) Note. GDS, geriatric depression scale; GDA, general depressive affect; LS, life satisfaction; W, withdrawal. Data were shown as β (95% CI). In the linear regression models, CRP level were transformed to log (X) and included as independent variable; and GDS, GDA, LS, and W scores were transformed into log (1+Y) values and included as dependent variable, when scores at follow-up were investigated. *P < 0.05. Table 4. Associations of baseline CRP levels with scores of GDS and its dimensions
-
This study revealed that general, rather than abdominal, obesity was positively associated with an increased risk of incident depression and worsening depressive symptoms in older adults, which was consistent with the findings of other studies. Previous studies have reported that increased BMI is predictive of a chronic course of depression [13] and that obese people have higher levels of depressive symptoms than those with normal weight [26]. One meta-analysis review revealed that obese adults have a 23%–36% increased risk of self-reporting depression symptoms as compared with non-obese subjects [27], and a Mendelian randomization study with a large sample found that a high BMI was strongly associated with a higher risk of depression and likely to have a causal role in the relationship [28].
However, there were some inconsistent results, which suggested that obesity was a protective factor for depression [29, 30]. A meta-analysis conducted by Yu et al. also concluded that older adults who were overweight and obese, defined by BMI, were less likely to be depressed than those with normal weight [31], supporting the "jolly fat" hypothesis. One possible explanation for this inconsistency is the differences in age, socioeconomic status, ethnicity, and culture [32].
An interesting finding in the present study was that obesity was associated with an increased risk of depression in older male adults alone, which was consistent with previous studies that found that older men with obesity had a 31% increase in the risk of depression [33], and no significant associations between depression and obesity based on BMI and WC were observed in Chinese female adults [34]. In older females, adipose tissue is the primary source of estrogen production [35], and the levels of estrogen in obese older women are much higher than those in non-obese women, and estrogen can help decrease the risk of depression in females [36, 37]. A higher level of estrogen may partly offset the risk of depression from obesity, leading to a less pronounced association between obesity and depression in older adults. However, other studies conducted in both American and Korean adults concluded that a positive association between obesity and depression was observed in women but not in men [38, 39], in which the mean age of subjects was < 60 years; therefore, the age differences of participants may elucidate the gender differences in the results of different studies.
We did not observe a relationship between abdominal obesity and worsening depressive symptoms or the incidence of depression, which was consistent with one meta-analysis [31] and a 10-year follow-up study that focused on older adults [40]. Some studies have concluded that abdominal obesity was positively associated with depression; however, majority of these studies were conducted in Western countries [41], perhaps because of ethnic differences that confounded the relationship between depression and abdominal obesity [42].
The current study showed that CRP levels were more likely to be higher in obese older adults, which was consistent with other studies that reported higher levels of CRP in obese people than in normal or lean people [43]. Obesity may cause metabolic disturbances associated with increased levels of subclinical chronic inflammation, such as increased serum CRP levels [44]. CRP was thought to be a candidate biomarker for depression and is commonly elevated in the serum of patients [45]. We found that the risk of high CRP levels did not increase in the overweight group, which partly explains why being overweight was not significantly associated with depression.
Interestingly, we also observed that increased CRP levels were negatively associated with life satisfaction, a specific dimension of depression but not with the overall GDS score. Previous studies have also revealed that increased CRP levels were strongly associated with reduced quality of life [46] and life satisfaction [47] but not with emotional symptoms [15]. Chronic low-grade inflammation may be a biological mechanism underlying depression. Long-term chronic inflammation can lead to damage and dysfunction of neuronal networks [48] and an inflammatory response can result in an overactive hypothalamic-pituitary-adrenal axis and neurodegeneration, leading to depression [49]. However, the relationship between psychiatric disorders and metabolic syndrome is complex [50], and leptin resistance may be another mechanism by which obesity leads to depression [32]. A previous study showed that downregulation of leptin/LepRb signaling may be associated with depression-like behavior in obese rats [51].
The strengths of the current study are as follows. First, this was a 3-year prospective cohort study, which can better explore the relationship between obesity and depression. Second, both general and abdominal obesity were investigated, and many confounding variables were adjusted for. Finally, we investigated the possible role of chronic inflammation in the relationship between obesity and depression. However, there were also several limitations. First, the criteria in China for obesity status were used, meaning that the results could not be generalized to other ethnic groups. Second, depressive symptoms were self-reported using the GDS and not clinically interviewed, which may introduce some recall bias; however, the GDS was widely used in community-dwelling older people and has good reliability. Finally, we had no data on antidepressant drug treatment, whereas obesity was shown to be related to the incidence of depression among those free of depression at baseline, which meant that antidepressant drugs were less likely to be a major source of confounding.
-
Our findings suggest that general obesity, but not abdominal obesity, is associated with worsening depressive symptoms and incident depression, which can be partly explained by the systemic inflammatory response defined by CRP levels. Interventions for obesity and its underlying correlations may be beneficial for the prevention and treatment of depression.
HTML
Study Subjects
Depression Assessment
Assessment of Obesity
Assessment of Systemic Inflammation and Baseline Covariates
Statistical Analysis
CONFLICT OF INTEREST The authors declare no conflict of interest.







 Quick Links
Quick Links
 DownLoad:
DownLoad: