-
Pancreatic cancer, which develops rapidly, is a common type of malignant tumors found in the digestive tract. According to the latest data from the American Cancer Society in 2022, pancreatic cancer ranks as the fourth leading cause of cancer death for new-onset cancers globally, the tenth for men, and the seventh for women. Despite rapid advances in precision medicine and improved survival rates for other types of cancer, the current outcomes of pancreatic cancer treatment regimens remain poor, with a 5-year overall survival rate of 11% and a 1-year survival rate of less than 20%[1]. Surgery and chemotherapy remain the most common treatment options for Pancreatic Cancer (PAAD). Because of high mortality rates, it is imperative to explore the genetic events in cancer and develop new, more effective targeted therapies. Most current cancer treatments including chemotherapy, radiation, and immunotherapy kill cancer cells by inducing apoptosis. Evading apoptosis is a common feature of all cancers, and many molecular mechanisms have evolved to resist apoptosis, especially in PAAD.
Copper ions, which are essential micronutrients, are found in extremely low concentrations in mammalian cells; however, their redox activity may damage the cells. If the intracellular concentration of copper ions exceeds the threshold required to maintain homeostasis, it can become cytotoxic[2]. In recent years, copper, platinum, and iron have been extensively studied as raw materials in the development of drug delivery systems, showing promising prospects for a range of anticancer purposes[3]. Many potential mechanisms for utilizing the biological functions of copper ions to treat cancer have also been investigated[4]. However, the role of copper in pancreatic cancer remains unclear. In the present study, we aimed to identify cuproptosis-related genes associated with clinical outcomes in PAAD, and constructed and validated a risk assessment model for PAAD based on the association of cuproptosis-related genes with clinical characteristics; we demonstrated its stability and accuracy in both the training and validation datasets, and highlighted the value of cuproptosis for prognosis in PAAD. We also studied the mechanism of action of cuproptosis-related genes by enrichment analysis. These efforts may help develop better treatment strategies in the future.
To investigate the relationship between cuproptosis-related genes and the development of pancreatic cancer tumors, we used The Cancer Genome Atlas (TCGA)-PAAD data to determine the expression levels of 49 cuproptosis-related genes in tumor and normal specimens and found that 24 genes were significantly differentially expressed (P < 0.05).
To further investigate the association between tumor survival time, clinical outcomes, and the 24 differentially-expressed genes, we used median grouped- Kaplan-Meier (KM) survival analysis and univariate Cox regression analysis; in order to make the screening results more accurate, we chose overall survival (OS), disease-specific survival (DSS), disease-free survival (DFI), and progression-free interval (PFI) as survival time for analysis, and selected the best λ value of evaluation index. Based on the results, we selected LIAS, DLAT, CCDC22, MT2A, MAP1LC3A, LIPT1, SNHG8, SNCA, and ACE for further analysis.
To screen the clinical features that affect the survival time of neoplasms, we performed Cox regression analysis on 17 clinical features in TCGA-PAAD data and found that sex, neoplasm histologic grade, pathologic stage N, and the presence of residual tumors had significant effects on the survival time of neoplasms.
We selected these four relevant clinical variables for Cox regression analysis and separately included the nine genes selected using least absolute shrinkage and selection operator (LASSO) to confirm whether an individual gene was meaningful in multivariate Cox regression analysis. Finally, we selected three significant genes with OS as the survival time. The expression of the risk score was as follows:
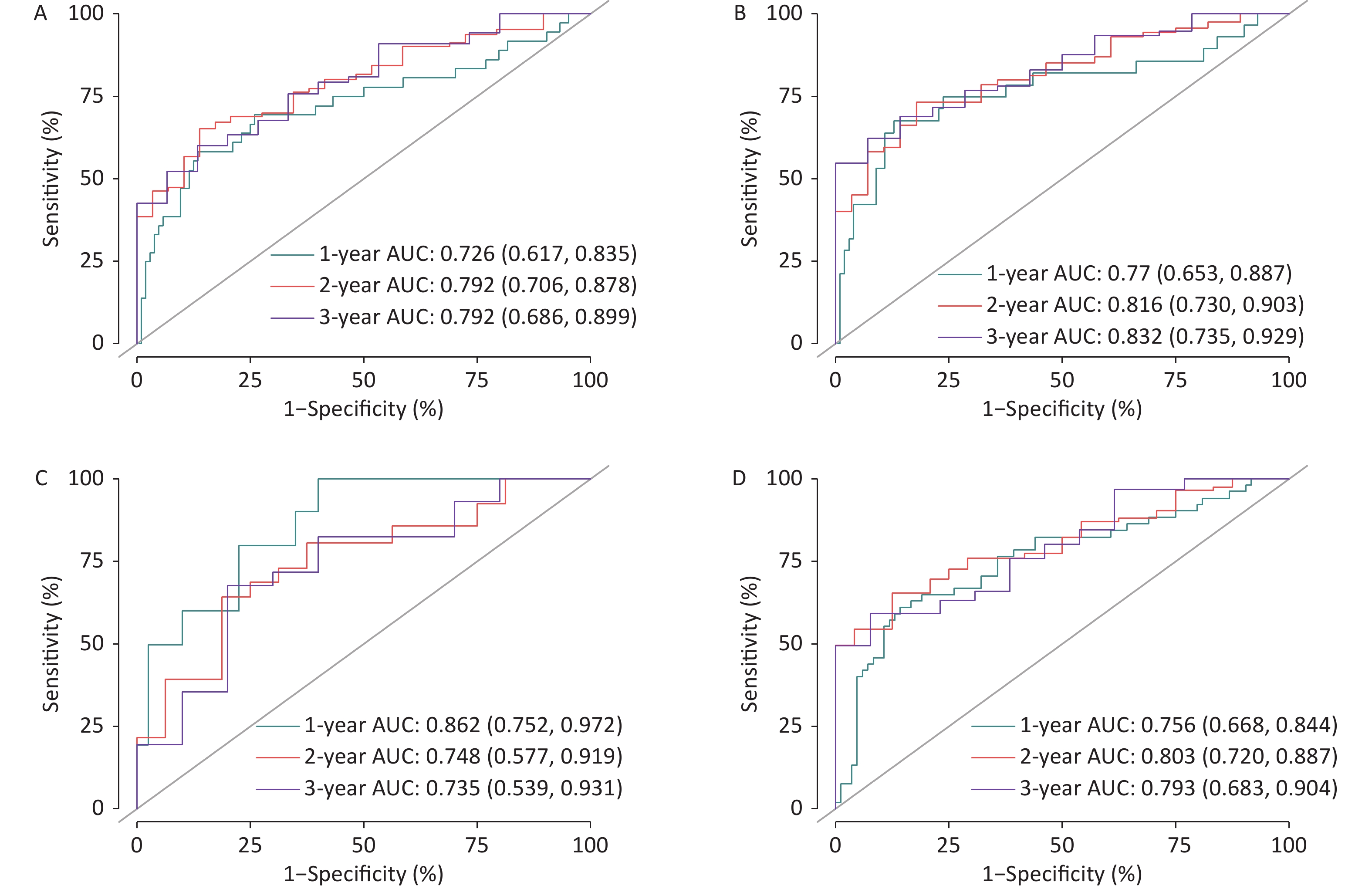
$$\begin{aligned} risk-score=&- 0.8675 \times LIPT1+0.1906 \times MT2A\\ &- 0.2231 \times SNCA \end{aligned} $$ (1) Subsequently, we constructed a PAAD risk assessment model using the risk score and four clinical features that significantly affected the survival time of patients with neoplasms: sex, neoplasm histologic grade, pathologic stage N, and residual tumor presence. Figure 1 indicates the ROC curves to predict the sensitivity and specificity of 1-, 2-, and 3-year survival according to the PAAD risk assessment model.
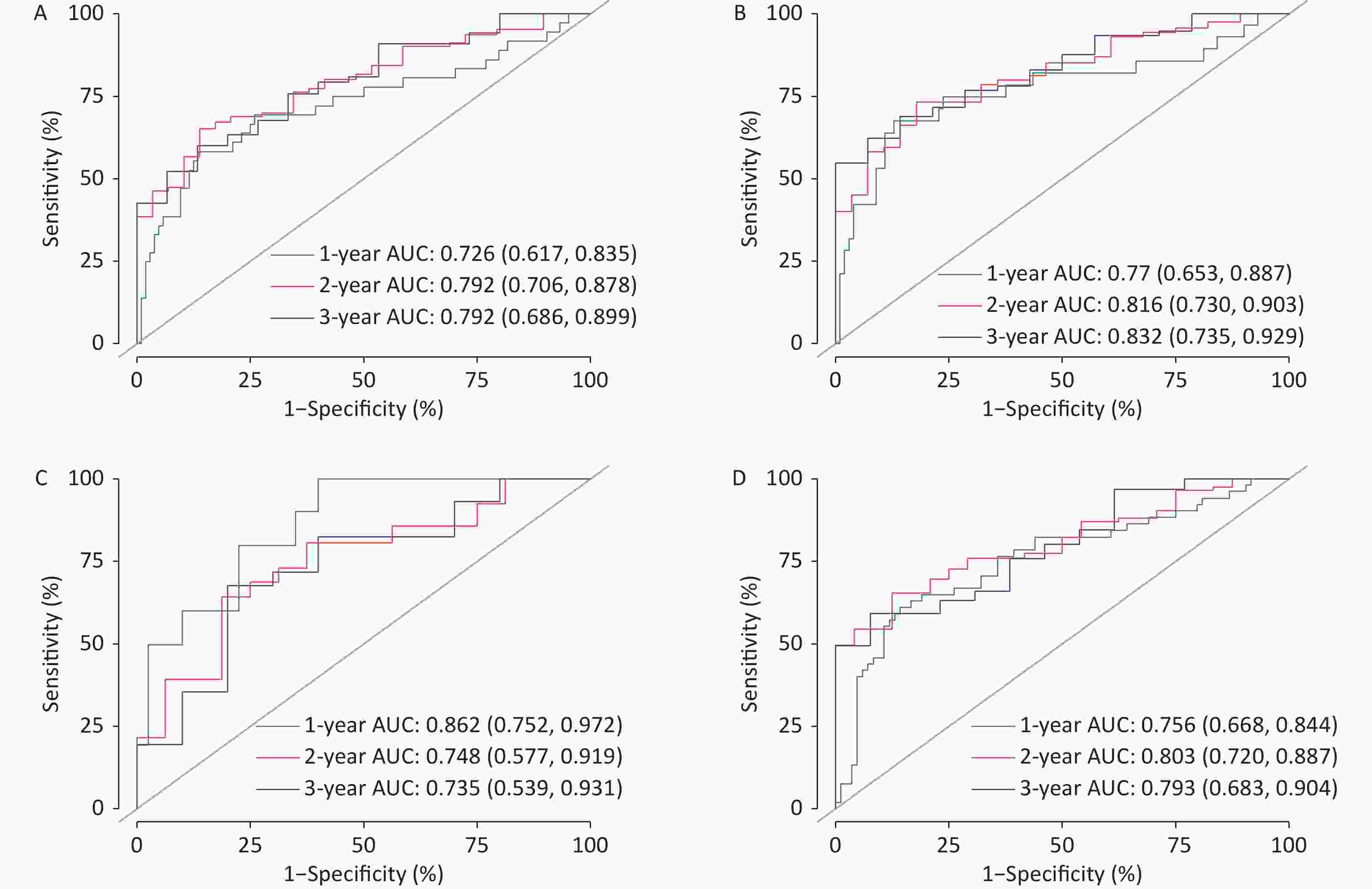
Figure 1. Receiver operating characteristic (ROC) curve for overall survival (OS) (A), disease-specific survival (DSS) (B), disease-free survival (DFI) (C), and progression-free interval (PFI) (D).
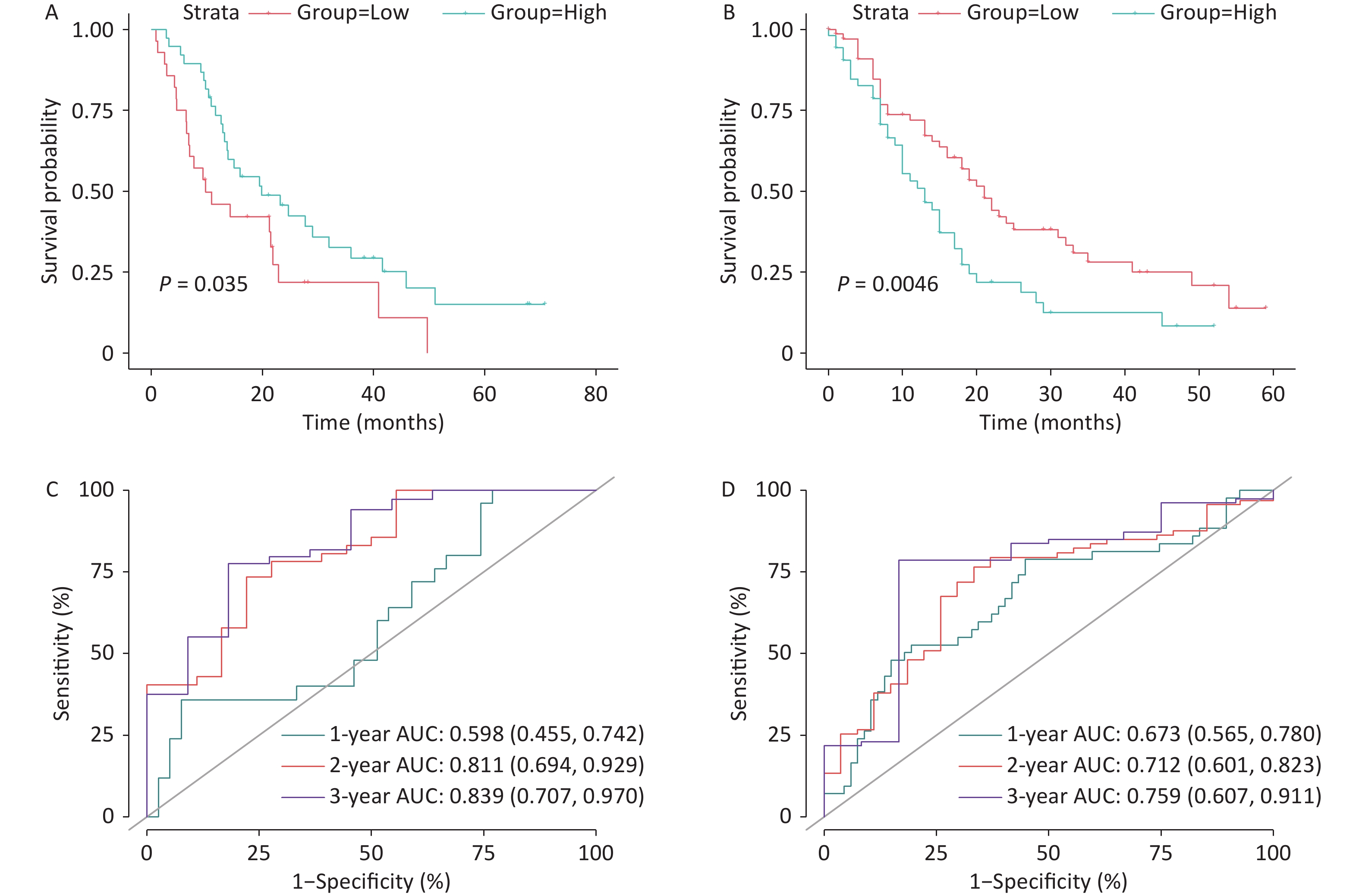
According to survival analysis results, the higher (H)-risk score group had a shorter survival time than the lower (L)-risk score group, both in the training and external validation datasets. In the TCGA-PAAD data set, the median survival time was 15.8 months for the H-RISK group and 23.4 months for the L-risk Group; Cox regression analysis showed a hazard ratio (HR) of 2.72 (95% CI) for the H-risk group compared to the L-risk group. The model showed good accuracy in multivariate Cox regression analysis of both datasets. As it is depicted in Figure 2, the model also showed satisfactory predictions in the external validation dataset (GSE62452: area under the curve (AUC) for 1, 2 and 3 years were 0.598, 0.811, and 0.839, respectively; GSE71729: AUC for 1, 2 and 3 years were 0.673, 0.712, and 0.759, respectively).
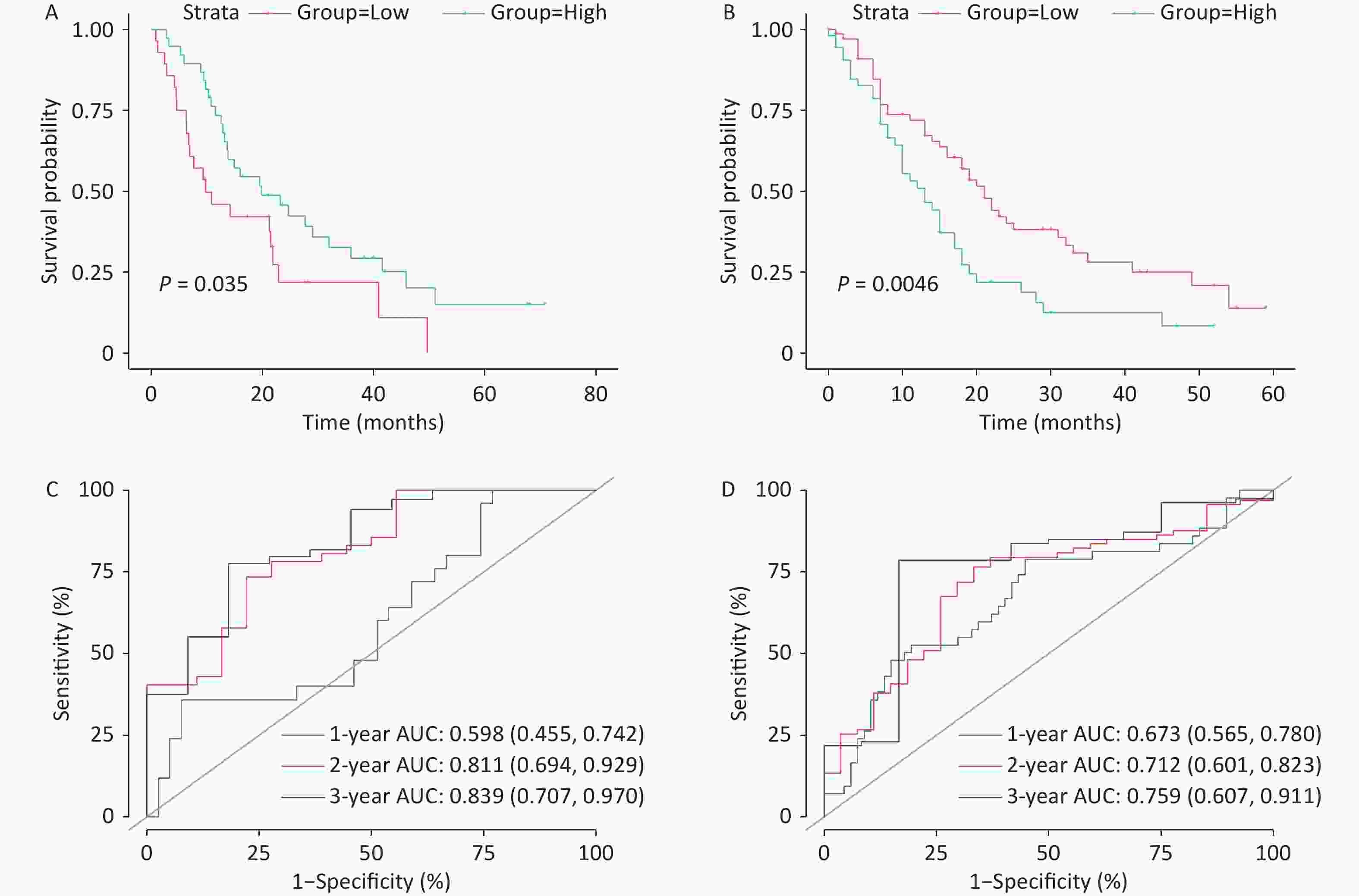
Figure 2. Survival analysis plot (A), receiver operating characteristic (ROC) curve (C) for GSE62452; survival analysis plot (B), ROC curve (D) for GSE71729.
To explore the possible biological pathways in patients with different risk scores, we compared gene expression levels in the H-risk score group with those in the L-risk score group using Kyoto Encyclopedia of Genes and Genomes (KEGG) and Gene Ontology (GO) analyses for 1,613 differentially expressed genes; the results are shown in Figure 3.
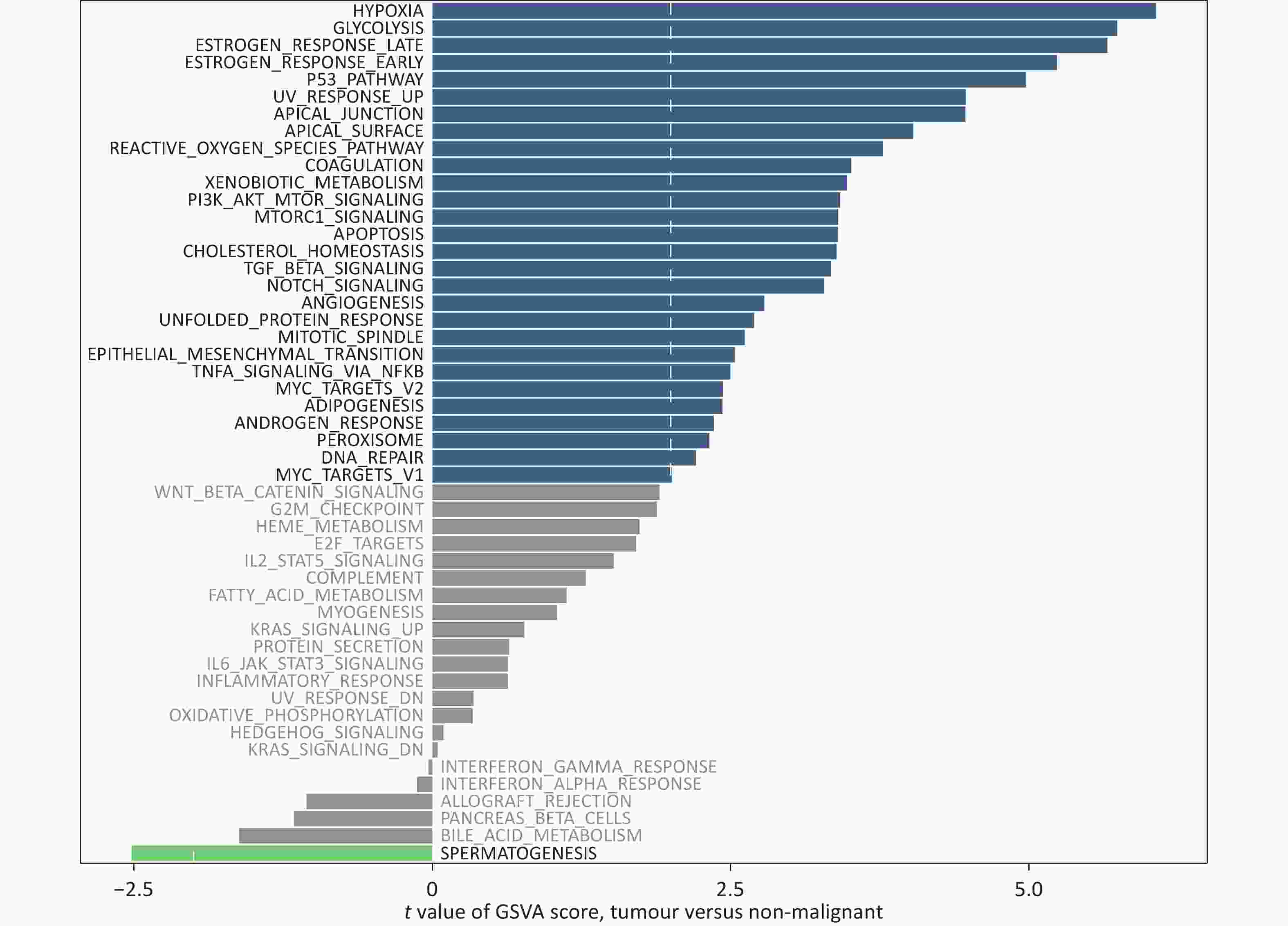
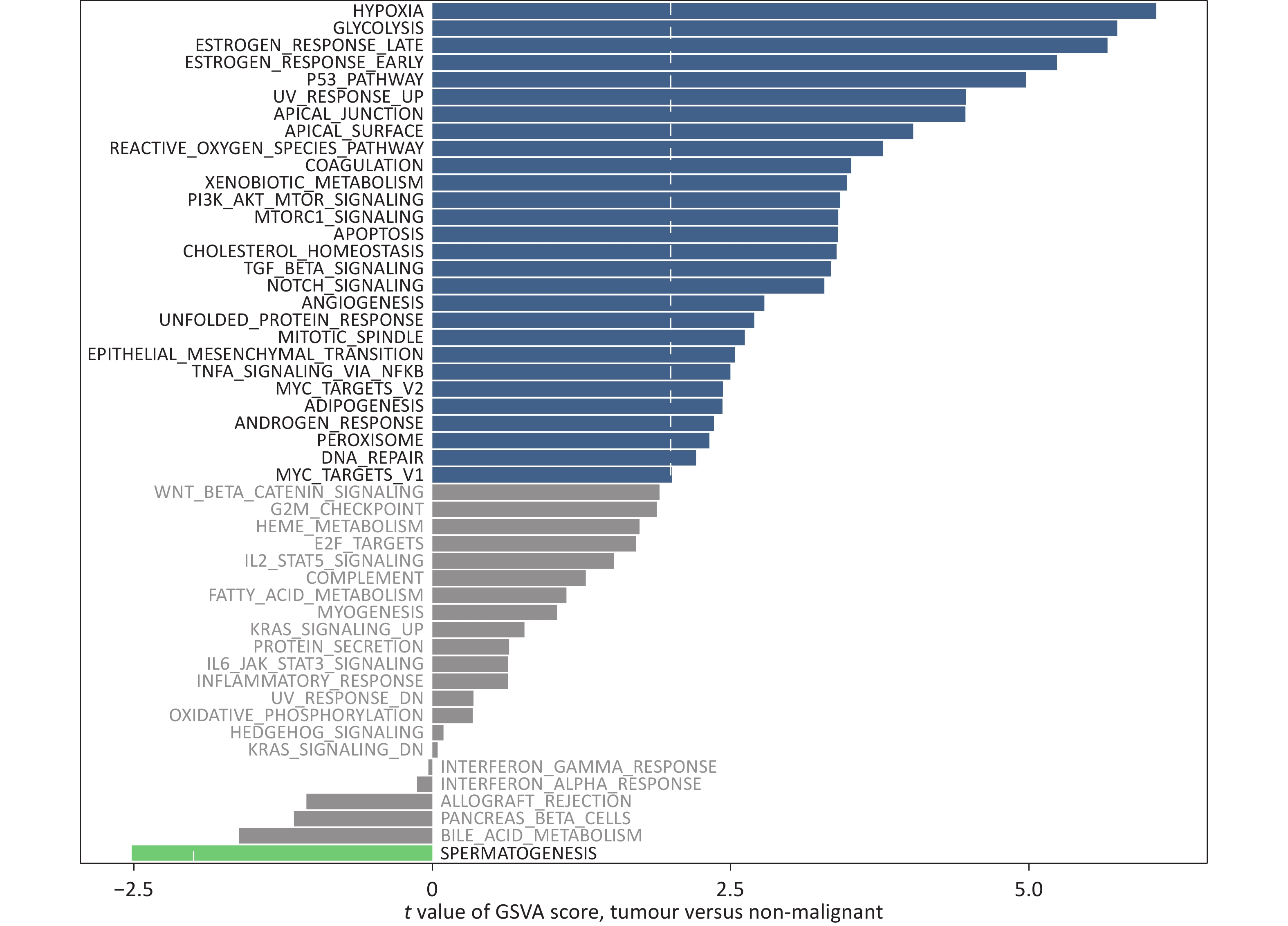
Figure 3. Gene set variation analysis (GSVA) of hallmark pathways in The Cancer Genome Atlas (TCGA).
The 1,613 differentially expressed genes had significant effects on focal adhesion, proteoglycans in cancer, the PI3K-Akt signaling pathway, the MAPK signaling pathway, and human papillomavirus infection. Furthermore, differential analysis of the gene set variation analysis (GSVA) scores between the H- and L-risk groups was performed. We compared the enrichment pathways of differentially expressed genes in the two groups and found that the HYPOXIA, GLYCOLYSIS, and ESTROGEN RESPONSE LATE pathways were mainly enriched in patients in the H-risk group, whereas the SPERMATOGENSIS pathway was mainly enriched in the L-risk group.
In this study, we focused on patients with different cuproptosis phenotypes associated with PAAD prognosis and aimed to describe their integration for clinical application and potential molecular mechanisms. Given the complexity of tumor biology, we recognize that it is not sufficient to predict clinical outcomes on the basis of a single gene or clinical feature alone; three genes (LIPT1, MT2A, and SNCA) and four clinical features (gender, neoplasm histologic grade, pathologic stage N, and residual tumor presence) that significantly affected the survival time of neoplasms were found to be potential diagnostic biomarkers. Receiver operating characteristic (ROC) maps were constructed and validated to predict the actual 1-year, 2-year, and 3-year survival of patients with pancreatic cancer, providing clinicians with a new means of predicting prognosis.
Lipoyltransferase 1, encoded by LIPT1, transfers lipoate to the E2 subunits of the 2-ketoacid dehydrogenases[5]. Thus, deficiency in the LIPT1 homolog could lead to decreased lipoylation of the E2 subunits. LIPT1 deficiency also suppresses TCA cycle metabolism. LIPT1 supports lipogenesis and balances oxidative and reductive glutamine metabolism in the functional assessment. LIPT1 deficiency has been reported in embryonic demise, early death, and leigh-like encephalopathy cases, such as early infantile epileptic encephalopathy, Leigh disease, secondary pyruvate dehydrogenase complex deficiency, and fatal lactic acidosis. Yuanbin et al. found that LIPT1 was among the genes correlated with a favorable prognosis in patients with urothelial cancer through analysis of the Pathology Atlas. Overexpression of LIPT1 in bladder cancer cell lines inhibits cell migration to some extent, but has no effect on cell viability. However, the mechanism underlying the regulation LIPT1 during cell migration remains unknown. Moreover, LIPT1 expression positively correlated with PDL1 expression and negatively associated with Treg infiltration. GSVA of LIPT1-upregulated genes revealed enrichment in some immune response-related pathways; hence, LIPT1 might regulate these pathways, such as IFNγ and IFNα to enhance the response to immunotherapy.
Mammalian metallothionein-2A (MT2A) is associated with autophagy regulation and apoptosis, meta homeostasis, detoxification, oxidative stress, immune defense, cell cycle processes, and cell proliferation, differentiation, and angiogenesis[6]. MTs are involved in many biological processes, including oxidation, cellular proliferation, differentiation, invasion, and carcinogenesis[7]. Relevantly, MT2A has the potential to control MAPKs and play a crucial pathophysiological function in anti-oxidation, anti-apoptosis, and anti-inflammation in various human carcinoma cases. High MT2A expression is significantly associated with aggressive pathological features of upper tract urothelial carcinoma (UTUC), such as tumor stage, lymph node metastasis, high tumor grade, vascular invasion, and perineural invasion. Gene coexpression analysis showed that MT2A overexpression promoted UC progression through complement activation. High MT2A expression is associated with aggressive features of UC and is an independent predictor of tumor metastasis and patient survival. Collectively, these studies demonstrate the importance of MT2A as a potential therapeutic target in PAAD.
SNCA mutant neurons showed mitochondrial dysfunction, oxidative stress, lysosomal swelling, and increased autophagy[8]. Ultimately, these multiple cellular stresses lead to aberrant excitability, altered neuronal activity, and cell death. It was found that the decrease of α-synuclein expression in dopaminergic neurons led to ferroptosis escape, and increased α-synuclein expression in small molecule-derived neuronal precursor cells in patients with SNCA leads to increased vulnerability to lipid peroxidation and ferroptosis.
According to our research, the poor OS prognosis of PAAD patients with different expression profiles of cuproptosis-related genes may be related to focal adhesion, proteoglycans, the PI3K-Akt signaling pathway, the MAPK signaling pathway, and the human papillomavirus infection pathway, or to the transmembrane transport, cell homeostasis, and transport of copper ions, which may affect the prognosis of patients with PAAD.
However, our study has some limitations. First, our study was retrospective, and a more convincing prospective study is required to validate our results. Second, molecular understanding should be validated by functional experiments between the cuproptosis-related genes and the three risk-score genes to promote further understanding of cuproptosis.
With the advent of new therapies for PAAD, it will become increasingly important to identify which patients do not benefit from current therapies and which may need to be treated early with these new approaches. The aim of our study was to determine whether the expression of cuproptosis-related genes predicts survival in patients with PAAD, which can be easily measured. To do this, we assessed the prognostic significance of 49 genes selected based on previous reports of their prognostic potential and our own analysis of available microarray data. The results of this evaluation allowed us to design a 3-gene model to predict OS in patients with PAAD.
In summary, this study constructed and validated a PAAD risk assessment model based on cuproptosis-related genes and clinical characteristics, which demonstrated stability and accuracy in both the training and validation datasets. The value of cuproptosis in the prognosis of PAAD was elucidated, and the possible molecular pathways involved in the model were discussed by means of enrichment analysis. An integrated evaluation of the risk score of each patient with PAAD is of great clinical importance and can be used to develop personalized immunotherapy strategies for these patients. Overall, the results of this study contribute to a better understanding of cuproptosis and to the development of better treatment strategies for the future.
A Risk Assessment Model for Pancreatic Cancer Based on Cuproptosis-related Genes and Clinical Characteristics
doi: 10.3967/bes2023.102
- Received Date: 2023-02-03
- Accepted Date: 2023-07-14
| Citation: | CHEN Yi Kai, WU Si Qian, LIU Wen Jun. A Risk Assessment Model for Pancreatic Cancer Based on Cuproptosis-related Genes and Clinical Characteristics[J]. Biomedical and Environmental Sciences, 2023, 36(8): 768-772. doi: 10.3967/bes2023.102 |








 Quick Links
Quick Links
 DownLoad:
DownLoad: