-
In recent years, air pollution has caused widespread concern around the world. According to a report used by the World Health Organization (WHO) in 2017, 93% of children worldwide, including 630 million children under the age of 5, were exposed to air pollution levels higher than the WHO Air Quality Guidelines[1]. In recent years, air pollution in China is severe. Although the government has taken strong measures, the current status of air pollution, especially PM2.5 pollution, does not inspire optimism. It has been shown that the average annual PM2.5 concentration in Beijing in 2018 was 52 μg/m3, and the number of days with a pollution concentration higher than 100 μg/m3 was 110, accounting for 1/3 of the year[2]. In winter, due to low temperatures, low air circulation, heating and other factors, there are more days with severe pollution than other seasons. Children are more mobile and breathe faster than adults, and children’s lungs and immune systems are immature and more sensitive to pollutants[3, 4]. Studies have shown that air pollution, especially fine particulate matter that has a diameter of less than 2.5 μm (PM2.5), has adverse effects on pulmonary function in children[5, 6]. The acute effect of this exposure needs to be given more attention. Studies in China, Japan, Mexico, Norway, and Poland have found that acute exposure to PM2.5 (4.24 μg/m3–143 μg/m3) has adverse effects on peak expiratory flow (PEF), forced vital capacity (FVC), forced expiratory volume in one second (FEV1), 25% forced expiratory flow (FEF25%), 50% forced expiratory flow (FEF50%), and 75% forced expiratory flow (FEF75%) in schoolchildren aged 9–16 years[7-13]. Abnormal pulmonary function is the root cause of such respiratory diseases as asthma in childhood and adulthood[14, 15]. Most children are healthy individuals and yet are still susceptible to air pollution. For this reason, the study of the effect of acute exposure to PM2.5 on pulmonary function of healthy schoolchildren has important application value for putting forward specific protective measures.
Pulmonary function, which is measured in terms of changes in lung volume, can provide valuable information on evaluating the effects of acute PM2.5 exposure on the lungs. There are two kinds of indexes of pulmonary function, large airway ventilation function indexes, that is, vital capacity (VC) and FVC[16], and small airway ventilation indexes, that is, FEV1/FVC, PEF, FEF25%, FEF50%, FEF75%, and 25%−75% forced expiratory flow (FEF25%–75%)[16, 17]. The rapid expiratory volume within one second of the maximum inspiratory level (FEV1), can be used to evaluate both large and small airway ventilation functions[17, 18]. Most studies included only a few representative pulmonary function indicators, such as FVC, FEV1, PEF, FEV1 and FEF25%–75%[19, 20], and the conclusions drawn in these studies were inconsistent. Li et al.[21] reviewed 20 panel studies on air pollution and lung function and found that FEV1 and PEF were the most common indicators used to evaluate children’s lung function. However, two studies found that acute exposure to PM2.5 can cause a reduction in both FEV1 and PEF, while one study found that acute exposure to PM2.5 only resulted in a reduction in PEF. Few studies compare these pulmonary function indicators at the same level. It is necessary to screen and evaluate these indicators together, and find out sensitive ones in children.
Ambient PM2.5 data from fixed air monitoring sites were usually used to evaluate the health effects of PM2.5 in most studies. For example, Qi et al.[22] used the daily PM2.5 concentration in 72 Chinese cities from 2013 to 2016 to evaluate and quantify the relationship between daily PM2.5 exposure and life expectancy, Qi et al.’s results suggested that reducing the concentration of PM2.5 can significantly extend life expectancy. This study had notable limitations in that they used monitoring station data, and were unable to obtain individual exposure data, which would have allowed more accurate assessment. So, it is still inaccurate to replace individual exposure concentrations with ambient air monitoring site data[23, 24]. Zhang et al.[25] compared PM2.5 individual exposure concentrations (using individual PM2.5 samplers) and fixed site ambient air monitoring concentrations over the same period, and they found a positive correlation between them, but the individual exposure concentration was lower than the fixed site ambient air monitoring concentration. Another study used time activity patterns and micro-environmental air monitoring data to estimate individual exposure levels[26], the results showed that short-term exposure to PM2.5 can cause respiratory inflammation and decrease FEV1 in 20 healthy 24-year-old adults at an average individual PM2.5 concentration of 169 μg/m3. Moreover, a review of 26 articles on air pollution exposure assessment in schoolchildren found that estimating individual exposure concentrations based on time activity data and micro-environmental measurement was the best way to assess schoolchildren’s air pollution exposure[27]. Though the accuracy order of different individual exposure concentration evaluation methods is as follows: individual sampler > time activity pattern and micro-environmental air monitoring > fixed site ambient air monitoring[4, 28], the time activity pattern and micro-environmental air monitoring data estimation method has lower cost than individual sampling, and the data accuracy is higher than that of fixed site ambient air monitoring, and could be a best compromise in evaluating individual exposure lever for schoolchildren.
In terms of controlling for confounding factors, schoolchildren have varying degrees of activity patterns, making it difficult to control for confounding factors, such as school attendance, travel, and micro-environments in their homes and classrooms.
This panel study aimed to determine the acute effects of exposure to PM2.5 on healthy schoolchildren’s pulmonary function. We performed the study in healthy schoolchildren in 4th−5th grade in a full-time boarding school in a district within Beijing, China, and we estimated individual exposure levels based on time activity patterns combined with school micro-environmental PM2.5 concentrations. During the study period, all students’ activities were limited to dormitories, classrooms, playgrounds, and the canteen, their activities and diets were controlled, and the influence of confounding factors, such as micro-environments of their homes and transportation were minimized.
-
The purpose of this study was to evaluate the impact of PM2.5 on lung function indicators within the same group under different pollution conditions, so we performed the survey three times in December 2018, March 2019, and April 2019. December 2018 showed low-pollution weather even though it was during heating season; March 2019 showed high-pollution weather also during the heating season; April 2019 showed high-pollution weather despite being during the non-heating season. Each survey was conducted for five days and included three parts: part 1 was exposure monitoring, including the hourly concentration of PM2.5 in classrooms, dormitories, the canteen, and playgrounds for five consecutive days during the survey; part 2 consisted of questionnaire surveys, including a parent questionnaire and a schoolchild questionnaire; part 3 was a physical examination on the last day of each survey, including height, weight, and pulmonary function. The study protocol was approved by the ethics review committee of the Chinese Center for Disease Control and Prevention (
No. 201803) and the Biomedical Ethics Committee of Peking University (No. IRB00001052-18089). Parents and schoolchildren were initially informed about the study, and all participants and their parents signed a written informed consent form. -
A total of 64 schoolchildren attend grades 4th−5th of the selected boarding school in a District of Beijing, China. The inclusion criteria were as follows: age between 9 and 12 years, willingness to participate in the study and commitment to complete the survey, and boarding at the school during the study. The exclusion criteria were as follows: respiratory infections, acute or chronic lung diseases before the survey; and leaving school during the study. A total of 51 children participated in our research, including 19 boys and 32 girls.
-
During the survey period, we placed PM2.5 measurement devices (Agris, WP6930S) in classrooms, dormitories, the canteen, and playgrounds for five consecutive days. All of the instruments were uniformly calibrated. The monitoring process was as follows: According to the schedule of students’ classes, the data was read every 40–60 min on average, and three calibrated direct-reading instruments were used in the same place each time, scattered within the same room far away from the doors and windows or at the center of playground, 1.5 m above the ground. Each instrument was reads three times, and the average value of nine reading across the three instruments was calculated and considered the average exposure concentration of the location during that period.
During the survey period, schoolchildren kept an activity log every day, where they recorded their individual daily indoor and outdoor activities and travel times.
According to the indoor and outdoor activity time of schoolchildren and indoor and outdoor PM2.5 concentrations, we estimated the individual daily exposure after time-weighted averaging with the following formula:
$${E_{\text{i}}} = \sum {{C_{\text{j}}}{t_{{\text{ij}}}}} /\sum {{t_{{\text{ij}}}}} ,$$ where Ei refers to the average individual exposure concentration of subject i to PM2.5 in micro-environment j, Cj refers to the concentration of PM2.5 in micro-environment j, and tij refers to the time subject i was in micro-environment j[28].
We calculated the 24-h individual daily exposure concentration from lag 0 d to lag 4 d and the average sliding individual daily exposure concentration from lag 0−1 d to lag 0−4 d. Lag 0 d referred to the day of physical examination; lag 1 d refers to 1 d before the day of physical examination; lag 2 d refers to 2 d before the day of physical examination; lag 3 d refers to 3 d before the day of physical examination; lag 4 d refers to 4 d before the day of physical examination; lag 0−1 d refers to the day of physical examination to 1 d before the day of physical examination; lag 0−2 d refers to the day of physical examination to 2 d before the day of physical examination; lag 0−3 d refers to the day of physical examination to 3 d before the day of physical examination; lag 0−4 d refers to the day of physical examination to 4 d before the day of physical examination. The daily exposure concentration on the day of physical examination day (lag 0 d) was calculated by taking the 15-haverage from 0:00 to 15:00 (midnight to 3:00 p.m.). We chose 15:00 because the physical examinations were ended at that time.
-
The parents questionnaire and the schoolchildren respiratory health questionnaire were based on the Respiratory History and Symptom Questionnaire (ATS-DLD-78-C) recommended by the American Thoracic Association[29]. The parents questionnaire was filled up by the child’s guardian and included the following: parents’ contact information, family ethnicity, child’s birth date, home address, child’s long-term disease status with respect to such conditions as bronchitis, asthma, history of respiratory allergies, and history of allergies to food, dust, detergents, and chemicals. The schoolchildren questionnaire was filled up by the children themselves, mainly to obtain information about recent respiratory symptoms, such as cough, sputum, sore throat, medication, and exercise. Medication referred to any use of anti-cold medicine in the past week. Exercise was divided into three levels: high, medium, and low, defined as having exercised more than 2 h per day, between 1 and 2 h, and less than 1 h. Before the start of the study, the parents questionnaire and the schoolchildren questionnaire were designed to exclude schoolchildren with acute and chronic respiratory diseases. After the end of the study (that is, the fifth day, Friday), the schoolchildren questionnaire was conducted again to collect medication and exercise information during the survey period.
-
Pulmonary function was performed using a portable pulmonary function testing device (SpirometerHI-801, Omron), the indexes included VC, FVC, FEV1, PEF, FEF25%, FEF50%, FEF75%, and FEF25%–75%. The detailed method was as follows. (1) Pulmonary function test parameters were selected. (2) For the FVC test, the subject covered his/her mouth, breathed calmly, inhaled as much as possible, then exhaled as much as possible, and returned to normal breathing after the last expiration. (3) For the FEV1 test, the subject covered his/her mouth, breathed calmly, inhaled as much as possible, and then expelled the air as quickly as possible. These pulmonary function tests need to be repeated at least three times. Comparing the three measurements, the difference between the maximum and minimum values of FVC must be less than 0.15 L (ΔFVC < 0.15 L), the difference between the maximum and minimum values of FEV1 must be less than 0.15 L (ΔFEV1 < 0.15 L), and the difference between the maximum and minimum values of PEF must be less than 0.67 L/s (ΔPEF < 0.67 L/s). The measurement result with the largest total value of FVC + FEV1 was selected as the final test result.
-
Basic information of schoolchildren, individual PM2.5 exposure data, and pulmonary function data were analyzed using basic statistical techniques. Continuous variables were expressed as mean (Mean, M) ± standard deviation (SD) or median and interquartile range (IQR) and were analyzed using the Analysis of Variance (ANOVA) or Wilcox symbol quality test, respectively. Categorical variables were expressed in terms of frequency and percentage. The Pearson chi-square test and Fisher’s exact test were used for statistical comparison among groups. Using PM2.5, gender, age, body mass index (BMI), allergy, medication, and exercise as fixed variables, survey times and ID as random variables, and pulmonary function indicators as dependent variables, a linear mixed-effects model was built to examine the influence on pulmonary function after different delays. The basic model was as follows:
$${Y_{{\text{ij}}}} = \sum {{\beta _{{\text{ij}}}}{X_{{\text{ij}}}}} + {\gamma _{\text{i}}}{Z_{\text{i}}} + {\gamma _{\text{j}}}{W_{\text{j}}} + u,$$ where Y refers to pulmonary function indicators VC, FVC, FEV1, FEV1/FVC, PEF, FEF25%, FEF50%, FEF75%, and FEF25%-75%, X refers to fixed variables PM2.5, gender, age, BMI, allergy, medication, and exercise, Z refers to the random variable ‘ID’, W refers to the random variable ‘survey time,’ β refers to the coefficient of the fixed variable, γ refers to the coefficient of the random variable, i refers to the i-th research object, j refers to the j-th survey, and u refers to the error.
Sensitivity analysis was conducted to evaluate the stability of the model. The effects of PM2.5 on all of the pulmonary function indicators were calculated with units of PM2.5 increase of 10 μg/m3.
All of the data were statistically analyzed using R 3.5.1 and the lme4 packages.
-
A total of 51 schoolchildren participated in the present study (Table 1); 37.25% were boys and 62.75% were girls, and they ranged in ages from 10.13−10.74 years old. BMIs were 18.12 −18.56 kg/m2, there were 8 schoolchildren who had histories of allergies to food, dust, detergents, or chemicals, 5, 4, and 6 schoolchildren had taken anti-cold medicine during the three survey periods, and more than 40% of schoolchildren exercised more than 2 h/d. The rate of exercise in the third survey was significantly different from in the other two surveys, P < 0.05.
Items First survey (n = 51) Second survey (n = 51) Third survey (n = 51) Age (mean ± SD) 10.13 ± 0.63 10.74 ± 0.84 10.74 ± 0.84 Gender (n, %) Boys 19 (37.25) 19 (37.25) 19 (37.25) Girls 332 (62.75) 332 (62.75) 332 (62.75) BMI (kg/m2, mean ± SD) 18.12 ± 3.68 18.44 ± 3.32 18.56 ± 3.45 Allergy (n, %) Yes 8 (15.69) 8 (15.69) 8 (15.69) No 43 (84.31) 43 (84.31) 43 (84.31) Taking anti-cold medicine (n, %) Yes 5 (9.80) 4 (7.80) 6 (11.76) No 46 (90.20) 47 (92.16) 45 (88.24) Average daily exercise (h/d), (n, %) > 2 22 (43.14) 24 (47.06) 25 (49.02)* 1−2 17 (33.33) 16 (31.37) 10 (19.61)* < 1 112 (23.53) 11 (21.57) 16 (31.37)* Note. n, sample size; SD, standard deviation. *Means significant difference compared with other groups, P < 0.05. Table 1. Basic characteristics of participants
-
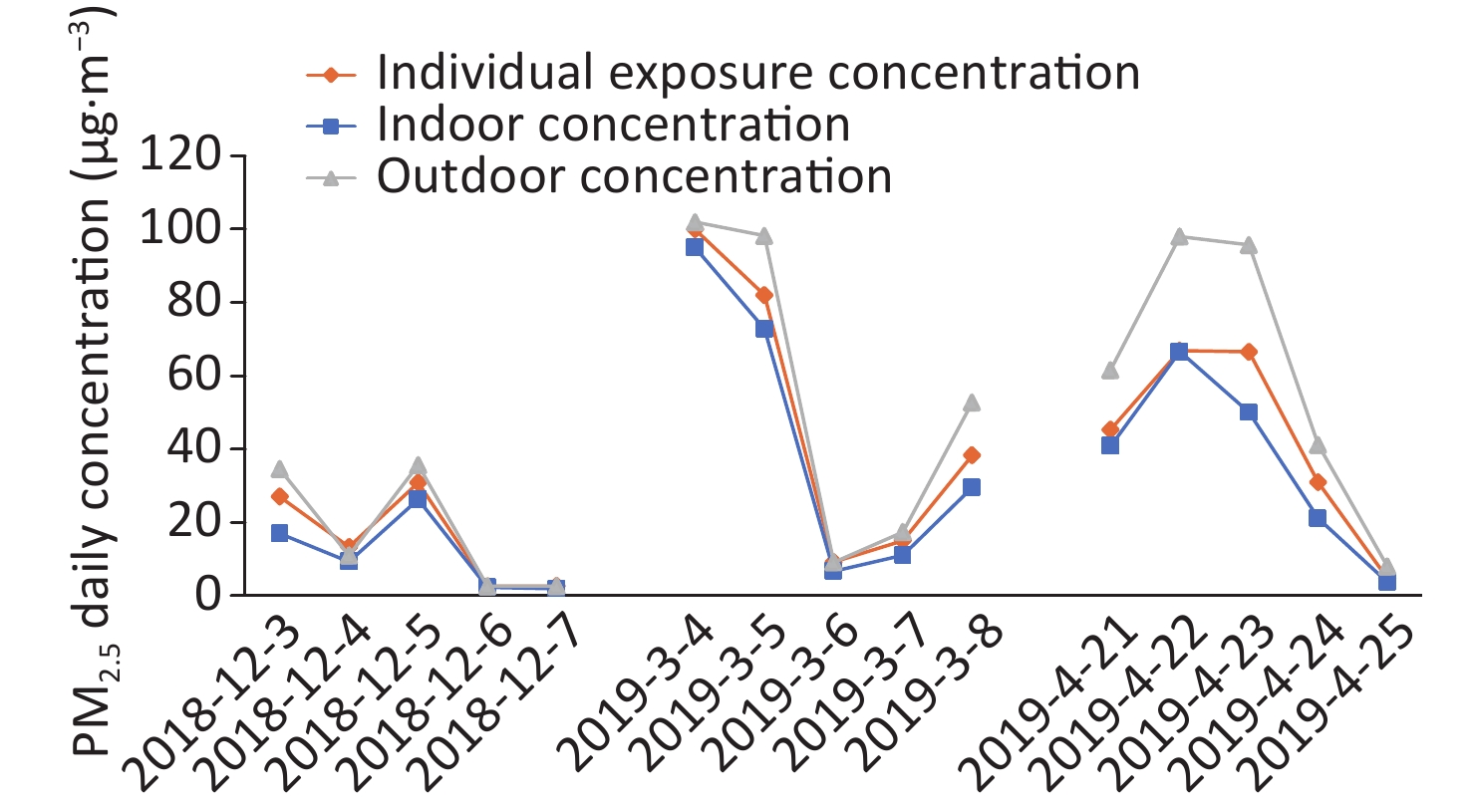
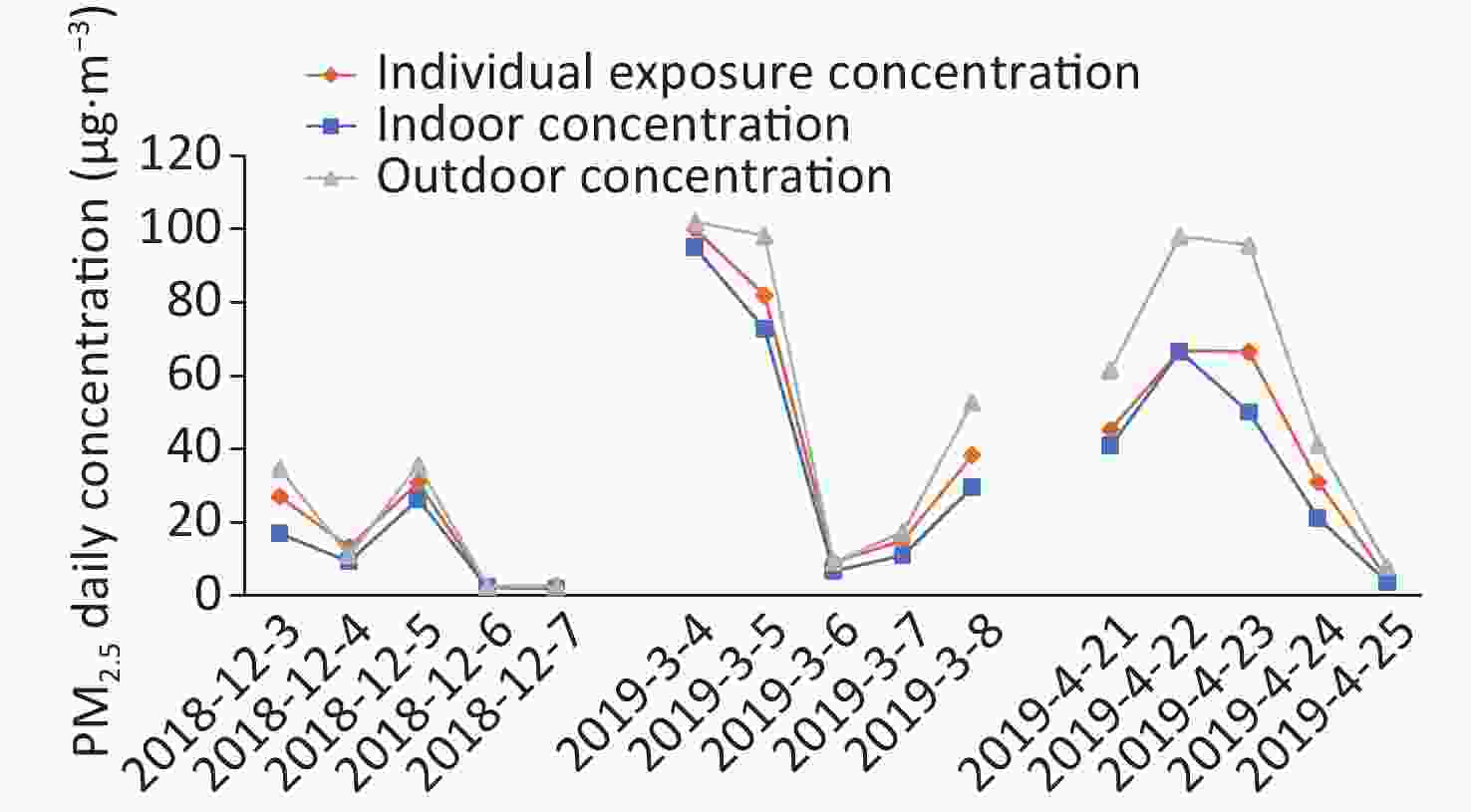
Figure 1 shows the average daily indoor and outdoor PM2.5 concentrations and individual exposure concentrations during the survey. As shown, during the first survey (December 3–7, 2018), the outdoor PM2.5 concentrations < 40 μg/m3, indicating good air quality. On some days of the second (March 4–8, 2019) and third (April 21–25, 2019) surveys, PM2.5 concentrations reached > 100 μg/m3, which were classified as slight pollution. A certain difference between indoor and outdoor concentrations was observed in the same time period. The individual PM2.5 exposure concentrations (calculated based on time activity patterns and micro-environmental PM2.5 concentrations) were between indoor and outdoor PM2.5 concentrations.
Table 2 shows the average individual exposure levels on different days, including daily average concentration on the day of physical examination, daily average concentration, and average sliding concentration 0 to 4 d before the physical examination. The highest exposure concentration was measured at lag 4 d of the second survey, and the lowest individual exposure concentration was measured on the day of the first pulmonary function test. The median of average individual daily PM2.5 concentrations at physical examination day was 6.00 μg/m3, the median concentration of lag 1 d to lag 4 d was 17.41 μg/m3, 30.75 μg/m3, 41.73 μg/m3, and 57.75 μg/m3, respectively, and on lag 0–1 d to lag 0–4 d it was 15.26 μg/m3, 18.7 μg/m3, 24.46 μg/m3, and 40.02 μg/m3, respectively.
Exposure
dayFirst survey (n = 51),
M (P25, P75)Second survey (n = 51),
M(P25, P75)Third survey (n = 51),
M (P25, P75)Total median,
M (P25, P75)Lag 4 d 17.15 (16.80, 17.15) 102.27 (100.39, 102.27) 57.75 (57.75, 57.75) 57.75 (17.15, 100.39) Lag 3 d 13.29 (13.29, 13.29) 41.73 (41.66, 41.73) 87.63 (87.63, 89.05) 41.73 (13.29, 87.63) Lag 2 d 30.75 (30.75, 30.75) 9.18 (9.18, 9.18) 65.95 (65.95, 67.42) 30.75 (9.18, 65.95) Lag 1 d 2.32 (2.32, 2.32) 17.41 (17.41, 17.41) 24.51 (23.95, 24.51) 17.41 (2.32, 23.95) Lag 0 d 1.94 (1.94, 1.94) 29.50 (29.50, 29.50) 6.00 (4.00, 6.00) 6.00 (1.94, 29.50) Lag 0–1 d 2.14 (1.94, 2.32) 23.46 (17.41, 29.50) 15.26 (6.00, 24.51) 15.26 (2.14, 23.46) Lag 0–2 d 11.67 (5.67, 26.97) 18.70 (9.18, 26.97) 32.16 (23.95, 65.95) 18.7 (11.67, 31.79) Lag 0–3 d 12.08 (6.78, 30.76) 24.46 (17.41, 41.66) 46.03 (23.95, 87.63) 24.46 (12.08, 46.03) Lag 0–4 d 13.10 (6.78, 26.97) 40.02 (26.97, 100.39) 48.37 (24.51, 57.75) 40.02 (13.10, 48.37) Note. n, sample size; M, median; P25, lower quartile; P75, upper quartile. Table 2. Individual PM2.5 exposure concentrations (μg/m3)
-
Table 3 shows the mean and standard deviation of the three surveys of pulmonary function indicators. The first survey pulmonary function indicators, that is, VC, FVC, FEV1 and FEV1/FVC were significantly different from the other two surveys (P < 0.01). No significant difference was observed for other indicators.
Pulmonary function indexes First survey (mean ± SD) Second survey (mean ± SD) Third survey (mean ± SD) VC (L) 2.06 ± 0.38* 2.44 ± 0.58 2.34 ± 0.35 FVC (L) 1.95 ± 0.39* 2.17 ± 0.43 2.22 ± 0.38 FEV1 (L) 1.80 ± 0.34* 1.86 ± 0.38 1.94 ± 0.37 FEV1/FVC (%) 0.93 ± 0.08* 0.85 ± 0.10 0.87 ± 0.09 PEF (L/s) 3.36 ± 0.91 3.39 ± 1.02 3.48 ± 0.81 FEF75% (L/s) 1.49 ± 0.44 1.28 ± 0.52 1.46 ± 0.52 FEF50% (L/s) 2.59 ± 0.71 2.44 ± 0.72 2.53 ± 0.73 FEF25% (L/s) 3.12 ± 1.03 3.18 ± 0.96 3.21 ± 0.84 FEF25%–75% (L/s) 2.25 ± 0.75 2.15 ± 0.68 2.32 ± 0.66 Note. SD, standard deviation; *P < 0.01, between this group and the other two groups. VC, vital capacity; FVC, forced vital capacity; FEV1, forced expiratory volume in one second; FEV1/FVC, expiratory volume in one second/forced vital capacity; PEF, peak expiratory flow; FEF25%, 25% forced expiratory flow; FEF50%, 50% forced expiratory flow; FEF75%, 75% forced expiratory flow; FEF25%–75%, 25%−75% forced expiratory flow. Table 3. Three measurements of pulmonary function
-
With lag 4 d exposure data, we excluded three independent variables (medication, allergy, and exercise) one by one for model sensitivity analysis (Table 4). We found that after excluding three independent variables separately, all of the pulmonary function indicators did not change significantly, indicating that the results have a high degree of confidence.
Variables VC (mL) FVC (mL) FEV1 (mL) FEV1/FVC (%) PEF (mL/s) FEF25% (mL/s) FEF50% (mL/s) FEF75% (mL/s) FEF25%−75% (mL/s) Basic model −37.29
(−54.51, −20.08)−32.55
(−50.26, −15.26)3.32
(−14.98, 21.61)−8.55
(−13.06, −4.04)−8.12
(−47.35, 31.10)−22.04
(−33.81, −10.28)−23.85
(−52.68, 4.99)−19.99
(−49.23, 9.24)−18.38
(−37.96, 1.20)− Medicine −37.97
(−55.26, −20.68)−32.69
(−50.43, −15.67)4.13
(−14.25, 22.51)−8.47
(−12.99, −3.96)−4.07
(−43.81, 35.66)−21.86
(−33.93, −9.79)−22.15
(−51.27, 6.97)−18.44
(−47.78, 10.91)−18.66
(−38.31, 0.93)− Allergy −37.79
(−55.10, −20.48 )−32.71
(−50.45, −15.13)3.98
(−14.57, 22.54)−8.03
(−12.56, −3.49)−6.21
(−45.55, 33.13)−21.94
(−33.78, −10.10)−22.87
(−51.79, 6.05)−18.30
(−47.56, 10.97)−18.67
(−38.46, 0.56)− Exercise −39.07
(−55.83, −22.31)−32.14
(−50.13, 15.69)4.90
(−13.75, 23.54)−8.30
(−12.68, −3.92)−2.08
(−40.33, 36.17)−22.10
(−33.99, −10.21)−21.70
(−49.68, 6.28)−17.38
(−45.70, 10.94)−18.56
(−38.11, 1.13)Note. The basic model independent variables were PM2.5, age, gender, BMI, exercise, allergies, and medication, and the dependent variables were indicators of pulmonary function. Allergies referred to history of allergies to food, dust, detergents, and chemicals. Each child’s long-term disease status such as bronchitis, asthma, history of respiratory allergies was excluded at the begin of the study. Medication referred to the situation of taking anti-cold medicine during the survey period. BMI was divided into three levels, < 18.5, 18.5−23.5, and > 23.5. All of the indicators were calculated based on each 10 μg/m3 increase in PM2.5. VC, vital capacity; FVC, forced vital capacity; FEV1, forced expiratory volume in one second; FEV1/FVC, expiratory volume in one second/forced vital capacity; PEF, expiratory flow; FEF25%, 25% forced expiratory flow; FEF50%, 50% forced expiratory flow; FEF75%, 75% forced expiratory flow; FEF25%–75% , 25%−75% forced expiratory flow. Table 4. Model sensitivity analysis (using lag 4 d data)
-
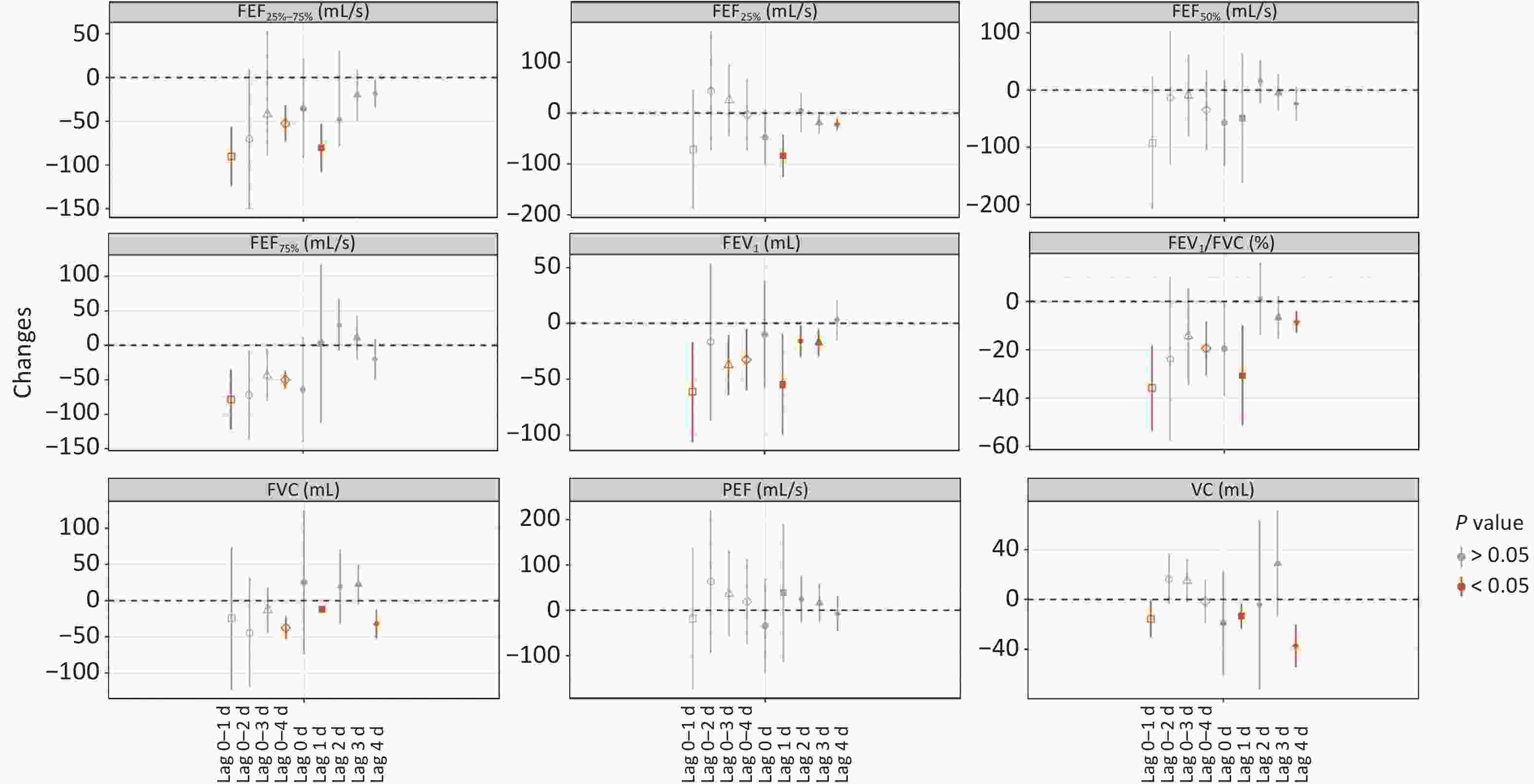
With the control of PM2.5, gender, age, BMI, allergy, medication, and exercise, we used the linear mixed-effects model to analyze the lag effects of individual PM2.5 exposure on pulmonary function. As shown in Figure 2, PM2.5 had no significant immediate effect on pulmonary function on the day of physical examination, but PM2.5 had a lagged effect on pulmonary function on lag days. Acute PM2.5 exposure can cause a decrease in VC, FVC, FEV1, FEV1/FVC, FEF25%, FEF50%, and FEF25%–75% on lag days; the largest declines were observed in FEF25%–75%, FEV1/FVC, FEF75%, and FEV1 on lag 0–1 d, 80.44 mL/s, 35.85%, 78.58 mL/s, and 61.34 mL, respectively, while the largest decreases were observed in FEF25% (83.68 mL/s) on lag 1 d, VC (32.34 mL) on lag 4 d, and FVC (37.76 mL) on lag 0–4 d.
-
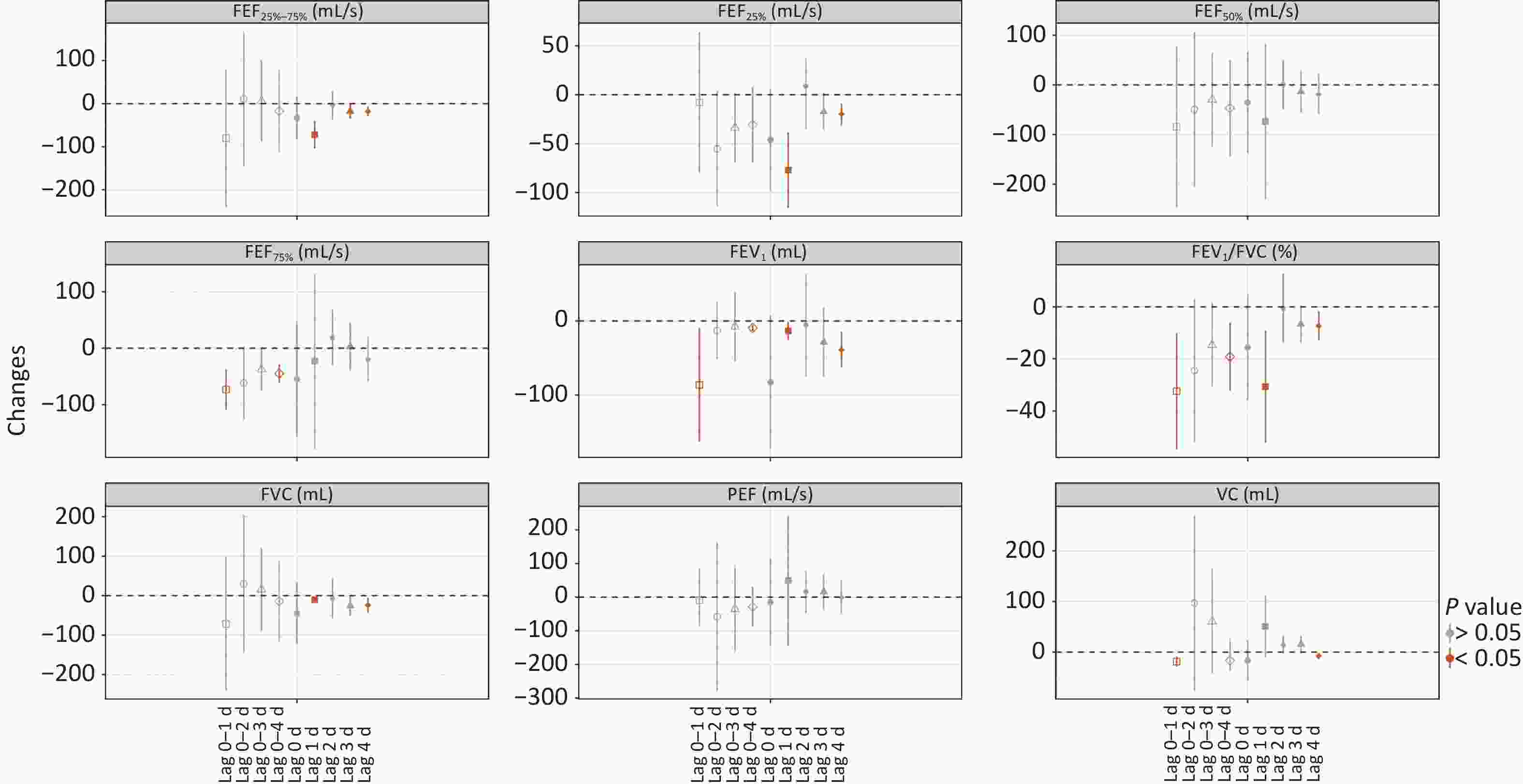
The subgroup analysis revealed that PM2.5 has inconsistent effects on pulmonary function between boys and girls (Figures 3–4), and the decline in most indicators was greater for boys than for girls. Each 10 μg/m3 increase in PM2.5 on the day of physical examination caused a decrease in FEV1 and FEV1/FVC in boys, that is, 62.26 mL and 25.85%, respectively. Among average sliding concentrations, each 10 μg/m3 increase in PM2.5 on lag 0–1 d caused a decrease in FEF25%–75% and FVC in boys of 99.92 mL/s and 82.11 mL, respectively; on lag 0–2 d and lag 0–3 d it caused a decrease in FEV1 in boys of 106.58 mL and 65.10 mL, respectively; and on lag 0–4 d it caused a decrease in FEF25%–75% and FVC in boys of 66.92 mL/s and 16.50 mL, respectively. No significant changes were found in girls at the same number of days. Among average daily concentrations, each 10 μg/m3 increase in PM2.5 on lag 1 day caused decreases in both boys and girls, in such indexes as FEV1, FVC, FEV1/FVC, FEF25%, and FEF25%–75%, and the decreases were more pronounced in boys than in girls. The same results were obtained for FEF25%–75% on lag 3 d, for FEV1, FEV1/FVC, FEF25%, and FEF25%–75% on lag 4 d. The changes in rest indexes were not statistically significant (Figures 3–4).
-
As schoolchildren have lower compliance than adults, and according to the Declaration of Helsinki, schoolchildren are not old enough to decide to participate in scientific studies. Therefore, for schoolchildren, especially young ones, the estimation of individual exposure to air pollutants not only has ethical problems but also faces a severe methodological challenge. We chose a boarding school, and used daily logs to record individual activities, which were combined with micro-environmental PM2.5 concentrations to estimate individual exposure concentrations as accurately as possible. Although this method is less reliable than individual exposure monitoring[28], a review of 26 articles mentioned above showed that it was the best way to assess schoolchildren air pollution exposure[27]. In particular, we controlled for multiple confounding factors; for example, (1) we chose full-time boarding school schoolchildren, limiting the scope of activities and minimizing the impact of travel and family-related factors, (2) classes participating in the study carried out activities in strict accordance with work–rest schedules and class schedules, and (3) three calibrated PM2.5 direct measurement instruments simultaneously monitored indoor and outdoor micro-environmental PM2.5 concentrations in the school. Therefore, the individual exposure concentrations estimated in our study are closer to the actual individual exposure levels than those estimated by conventional methods using time activity patterns and micro-environmental concentrations.
In addition, we compared the effects of the atmospheric monitoring data during the same period and the individual exposure concentrations estimated by time activity patterns and micro-environmental concentrations on the same pulmonary function index FEV1 (data not published). We found that each 10 μg/m3 increase of PM2.5 at the monitoring station caused a decrease in FEV1 of 53.66 mL, and the individual PM2.5 exposure concentration estimated by time activity pattern and micro-environmental concentration caused a decrease of 54.63 mL in FEV1 for each 10 μg/m3 increase in PM2.5, indicating that using fixed site ambient air monitoring data may underestimate the impact of PM2.5 on pulmonary function, at least not as accurate as the time weight concentrations.
-
Our study included nine pulmonary function indicators, including large and small airway indicators, allows us to evaluate the acute effects of PM2.5 on multiple aspects of pulmonary function. We found that the reduction in VC and FVC caused by PM2.5 on lag 1 d was less than that on lag 4 d, but the reductions in FEV1, FEV1/FVC, FEF25%, and FEF25%–75% were larger than on lag 4 d. Similar findings were found on lag 0–1 d compared with lag 0–4 d (excluding FEF25%), indicating that acute exposure to PM2.5 can reduce the large and small airway ventilation function at the same time. Short term exposure mainly affects the small airway ventilation function, and longer exposure times mainly reduce large airway ventilation. It has been found that PM2.5 could enter finer bronchial branches, capillary bronchi, and even alveoli, so it is more likely to deposit in small airways, causing them to react faster than large airways[3, 18]. A study of 182 asthmatic children in Canada found that FEV1 decreased by 0.73% for each 6.5 μg/m3 increase in PM2.5 on lag 1 d[30]. A study that pulmonary function measurements in healthy schoolchildren aged 13–14 were repeated seven times, showed that 8 h with a daily average PM2.5 concentration of 67 μg/m3 on lag 1 d was associated with a reduction in FEF25%, FEF50%, and FEF75%[7], indicating that small airway ventilation is more sensitive to acute PM2.5 exposure than large airway ventilation. The indicators that reflect large airway ventilation, such as VC and FVC, generally changed significantly after longer exposure. A birth cohort study including 1,058 healthy 8-year-old schoolchildren used land use regression and dispersion exposure modeling approaches to analyze the correlation between pulmonary function (FVC, FEV1, and PEF) and average annual PM2.5 concentrations from fixed site ambient air monitoring; the results showed that FVC and FEV1, large airway ventilation function indicators, decreased with increasing PM2.5, but PM2.5 had little effect on PEF, the small airway ventilation function indicator[31]. The above studies showed that VC and FVC could be used to evaluate the long-term effects of PM2.5 on pulmonary function, FEV1/FVC, FEF25%, and FEF25%–75% could be used to evaluate the acute effects of PM2.5 on pulmonary function, and FEV1, the most sensitive indicator among the nine indicators, could be used to simultaneously evaluate acute and chronic impact. In addition, studies have shown that PM2.5 can induce or promote airway hyperresponsiveness and airway inflammation through metabolic activation, inflammation, oxidative stress and genotoxicity[32]. This mechanism confirmed that PM2.5 has a certain correlation with abnormal lung function.
-
We found that PM2.5 concentrations on the day of physical examination had no effect on pulmonary function, but concentrations on lag 1 d to lag 4 d, lag 0–1 d, lag 0–3 d, and lag 0–4 d were associated with a reduction in VC, FVC, FEV1/FVC, FEF25%, FEF75%, and FEF25%–75%, suggesting that PM2.5 exposure has a delayed effect on schoolchildren’s pulmonary function. Xu et al.[13] used fixed site monitoring data and repeated pulmonary function tests four times with 86 schoolchildren, and analyzed the correlation between lag 1 d, lag 0–1 d, and lag 0–2 d sliding average PM2.5 concentration and pulmonary function indicators. They found that lag 0–1 d PM2.5 sliding average concentration was related to a reduction in FVC, FEV1, PEF, and FEF25%–75%. Zhang et al.[19] measured pulmonary function four times in 37 healthy adults and monitored PM2.5 concentrations at the same time; their study concluded that PM2.5 had a strong 1-d lag effect. Unlike our study, using time activity patterns and micro-environmental PM2.5 concentrations to estimate individual exposure concentrations, these two studies used fixed site monitoring data or monitoring data within the range of activity, but all three studies conclude that PM2.5 had a strong lagged effect on pulmonary function, and the effect could appear 1 d after exposure. Animal studies found that 6 h after dropping PM2.5 suspension into the trachea of mice, the ability of phagocytosis of macrophages in the PM2.5-exposed group was significantly lower than that in the control group[33], indicating that the occurrence of pulmonary inflammation could be detected 6 h after exposure, which also proves that PM2.5 has a lag effect on pulmonary function.
Moreover, we found that the effects of PM2.5 on pulmonary function could persist for many days. The effect of lag 4 d was second only to the effect of lag 1 d, and the effect of lag 0–4 d was second only to the effect of lag 0–1 d. However, the average individual exposure concentration of lag 4 d (57.75 μg/m3) was the highest, while that on lag 1 d was only 17.41 μg/m3. Similar results were obtained in other studies of acute exposure to pulmonary function in children; Chen et al.[4] analyzed the correlation between pulmonary function and the monitoring stations mean PM2.5 concentrations at lag 0–1 d and lag 0–2 d in 1,494 6–15-year-old schoolchildren. Although they did not control for confounding factors such as travel and family-related factors, their results indicate that although the concentration at lag 0–1 d (26.11 μg/m3) was lower than the concentration at lag 0–2 d (27.09 μg/m3), the lag 0–1 d effects (the reduction in FVC, FEV1, and MMEF) were stronger than the effects on lag 0–2 d. Similar results were obtained in healthy older people; Chu et al.[34] used fixed site monitoring data (PM2.5 exposure concentration between 10–100 μg/m3) and repeated pulmonary function tests 15 times with 20 elderly people without cardiopulmonary diseases, and found that lag 7 d concentrations were higher than lag 2 d concentrations, but lag 2 d had the greatest effect on FVC, FEV1, PEF, FEF25%, FEF50%, and FEF25%–75%. These results indicated that the effect of PM2.5 on pulmonary function might be affected by two factors. One factor is time; the effect could appear at lag 1 day, and then become weaker. The other is concentration; the higher the pollution, the longer the lag effect duration. This could explain why lag 4 d saw a higher concentration of pollution, but its effect weakened after 4 d of exposure, becoming even weaker than that of lag 1 d. Our study suggests that when pollution occurs, people not only need to take protective measures, such as wearing a mask when going out, closing doors and windows, and turning on an air purifier, but also need to pay attention to personal protection for a period of time after the pollution occurs.
-
Our subgroup analysis found that acute exposure to PM2.5 affected boys more than girls.
First, acute exposure to PM2.5 only has immediate effects on boys. Acute PM2.5 exposure on the day of physical examination can cause a decrease in FEV1 and FEV1/FVC in boys, suggesting that PM2.5 has immediate effects. Wang et al.[35] used individual exposure monitoring to repeatedly measure pulmonary function in 36 healthy college students in Shanghai. The individual PM2.5 exposure concentration was 35–48 μg/m3, and after controlling for confounding factors such as travel and activity, a decrease in FEV1 and FEV1/FVC was observed after 3–6 h of exposure, indicating that changes in pulmonary function changes could be observed after 3−6 h of acute PM2.5 exposure, consistent with our results, which was that PM2.5 has immediate effects. However, their study did not analyze the effects of gender differences, and did not observe the gender differences in the immediate effects.
Second, PM2.5 has a stronger lag effect on boys than on girls. We found that the increase in PM2.5 caused most of the pulmonary function indicators (FEV1, FVC, FEV1/FVC, FEF25%, and FEF25%–75%) to decline more in boys than in girls (Figure 3), indicating that boys are more sensitive to PM2.5 than girls, which is consistent with most studies[3, 8, 13, 36]. Gao et al.[3] used monitoring data from fixed sites near the school, controlled for mixed factors, such as weight and exercise, and they used multiple linear regression models to analyze the effects of PM on pulmonary function in 2,060 schoolchildren aged 8–10 years. They found that FEV1, FEF25%–75%, and FEF75% decreased with increasing PM, but this phenomenon was not observed in girls. Similar results were obtained regarding the effects of chronic PM2.5 exposure on pulmonary function. For example, Hwang et al.[36] used a multiple linear regression model to evaluate the association between annual average PM2.5 concentration and pulmonary function in 2,941 12-year-old pupils, and they found that FVC, FEV1, and FEF25%–75% of boys decreased with increasing PM2.5, but they did not find similar changes in girls. The reasons may be as follows. (1) The study subjects were 8–12 years old. In this age group, girls generally develop earlier than boys, and their lungs are relatively mature, so they are less affected by PM2.5 than boys[18]. (2) The inconsistent exercise intensity and the difference in activity levels between boys and girls may have led to different effects of PM2.5 on pulmonary function[37].
-
Our study has some strengths. First, our research concerns acute exposure to PM2.5 among healthy primary school students. Most of the current research focuses on people with diseases, but there has been little attention paid to large number of healthy students. Second, because it is not easy for elementary school students to cooperate with individual exposure concentration monitoring, most studies estimate exposure using monitoring station data and only make a rough estimate of outdoor concentrations. However, the time people spend indoors and outdoors differs, and the indoor and outdoor concentrations are also different. Our study was based on the time-weighted average individual exposure concentration calculated using the time activity model, considering the differences in indoor and outdoor concentration. The calculations regarding time spent indoors and outdoors and the activities performed in these places by each individual are more accurate than in most studies. Third, it is difficult to control confounding factors in repeated measurement design research. In the present study, we selected boarding school students, which gave us a population with a roughly consistent actions and diet, and avoided the impact of such factors as schooling and family, which makes our research results more convincing. Finally, most studies select only a small number of lung function indicators. We here considered nine lung function indicators (VC, FVC, FEV1, FVC/FEV1, PEF, FEF25%, FEF50%, FEF75%, and FEF25%–75%), accounting for assessment of the large and small airways, which is more comprehensive than most studies.
We wish to mention three minor limitations to our study. The sample size of this study was relatively small, we only obtained pulmonary function data from schoolchildren of one primary school, and the impact of other pollutants on pulmonary function has not been considered. Future studies should include different regions, different schools, and different age ranges, and the effects of more air pollutants on pulmonary function should be explored.
-
We chose a full-time elementary boarding school where schoolchildren had a limited range of activities in order to unify actions and diets and minimize the effects of confounding factors such as family-related factors, diet, and school trips. Drugs, allergy, and sports were controlled in the statistical model. We accurately estimated the individual PM2.5 exposure levels of schoolchildren using time activity patterns and micro-environmental concentrations, and we analyzed the acute impact of PM2.5 on nine pulmonary function indicators and studied the immediate and delayed effect of polluted weather. We found that acute PM2.5 exposure had a significant lag effect on pulmonary function, both on small airway indicators and large airway indicators. Boys’ pulmonary function was more sensitive to PM2.5 than girls.
Author Contributions Data curation, YANG Xiao Yan, HAN Feng, and WANG Qin; Formal analysis, YANG Xiao Yan; Funding acquisition, XU Dong Qun; Investigation, YANG Xiao Yan, WEN Bo, HAN Feng, WANG Chong, ZHANG Shao Ping, WANG Jun, and WANG Qin; Methodology, YANG Xiao Yan, WEN Bo, HAN Feng, WANG Qin, and XU Dong Qun; Project administration, YANG Xiao Yan, and WANG Qin; Resources, XU Dong Qun; Visualization, YANG Xiao Yan; Writing – original draft, YANG Xiao Yan; Writing – review & editing, YANG Xiao Yan, WANG Qin, and XU Dong Qun.
Conflict of Interest The authors of this study have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Acknowledgments We would like to express our gratitude to the teachers and students for their cooperation and dedication. At the same time, we thank GUO Xiao Xiao, YUAN Yuan, and DENG Fu Chang from Chinese Center for Disease Control and Prevention for their help in sample collection.
Acute Effects of Individual Exposure to Fine Particulate Matter on Pulmonary Function in Schoolchildren
doi: 10.3967/bes2020.086
- Received Date: 2020-04-08
- Accepted Date: 2020-06-12
-
Key words:
- PM2.5 /
- FEV1 /
- VC /
- PEF /
- FEF25%–75%
Abstract:
| Citation: | YANG Xiao Yan, WEN Bo, HAN Feng, WANG Chong, ZHANG Shao Ping, WANG Jun, XU Dong Qun, WANG Qin. Acute Effects of Individual Exposure to Fine Particulate Matter on Pulmonary Function in Schoolchildren[J]. Biomedical and Environmental Sciences, 2020, 33(9): 647-659. doi: 10.3967/bes2020.086 |










 Quick Links
Quick Links
 DownLoad:
DownLoad:


